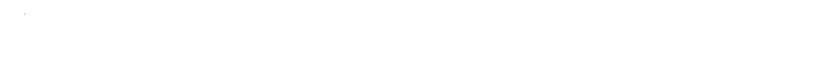Glucose: Past, Present, and What Lies Ahead
A Look Back at the Journey
Glucose landed on the map back in the early nineteenth century, with chemists breaking down honey and fruit juice to reveal this simple sugar at the very core. Early researchers didn’t have the luxury of high-end spectrometers or standardized lab equipment, so they relied on taste, basic crystallization routines, and a bit of luck. The industrial revolution pushed the need for affordable sweeteners. Factories started churning out glucose syrup by breaking down starch from wheat and corn. The process kept evolving, but the demand stayed the same—sweetness, a quick jolt of energy, and a cheap solution for both families and businesses. These practical moves in food manufacturing set the stage for the complex glucose production we see today.
Understanding Glucose as a Product
Glucose rarely stands alone on grocery store shelves; it shows up in granulated, liquid, and tablet forms. People know it as dextrose in the pharmaceutical aisles, or as a syrup in the food industry where it tweaks texture and draws out flavors. It serves as pharmaceutical-grade powder for diabetics, fuel for athletes, and filler in candies. Its short shelf life encourages manufacturers and pharmacists to safeguard quality, since any contamination can undermine its purity and safety.
Physical and Chemical Features
The stuff dissolves like a dream in water and packs a gentle flavor compared to sucrose. Under the microscope, those colorless crystals hide a C6H12O6 structure, a straightforward six-carbon molecule that holds just enough complexity to matter. It rotates polarized light, a neat trick appreciated by biochemists. While glucose withstands plenty once dissolved, heat or acidic conditions can caramelize it or flip it into other sugars. Its reactivity is a two-edged sword, offering versatility but calling for precise handling in production and use.
The Nitty-Gritty: Technical Specs and Labeling
Regulators keep a close eye on glucose, especially those barrels bound for hospital and food service. Producers stamp labels with batch numbers, purity percentages, synthetic or natural origin, and allergen status. In the US, the FDA and USP square off with their own standards, making sure nothing unsavory slips in. European markets often demand GMO statements, echoing growing consumer skepticism toward modified crops. On every container meant for clinical or laboratory work, specs line up to a level that doesn’t leave much to chance.
How Glucose Comes to Be
Most factories pull glucose from starch—corn wears the crown, but potatoes, wheat, and rice also step up. It starts with a slurry, heated and stirred until enzymes break everything down into liquefied sugars. After filtering and more processing, workers end up with pure glucose, ready for crystallization or kept as syrup. Over the years, some companies swapped harsh acids for gentle enzyme catalysts— a move backed by both cost savings and concerns over toxic byproducts. The whole approach skips high-tech trickery in favor of centuries-old wisdom, nudged forward by biochemistry.
Reactions and Chemistry off the Shelf
Glucose changes its tune in a heartbeat. Into a pot, mixed with nitrogen sources, it squares up as the main player in fermentation—beer, wine, and yogurt depend on it. Tossed in a test tube, it can link up with proteins to form glycosylated compounds—something of a hot topic in diabetes and metabolic research. Industry also turns it into derivatives like sorbitol and gluconic acid, using either microbe tricks or direct electrochemical tweaks. Its high reactivity helps, but specialists need to control temperature and pH to avoid piles of brown, degraded sugars that no bakery or IV bag wants.
What Folks Call It
Chemists recognize it as D-glucose, but most people call it grape sugar or blood sugar. Dextrose pops up in hospitals and gyms, where it kicks in fast for an energy boost. Candy makers stick with glucose syrup. These names reflect a spectrum of uses—from a sweet treat to a life-saving component of medical care.
Keeping Safe and Playing by the Rules
Consistent quality runs the show, especially where hospitals treat low blood sugar or athletes reach for rapid energy. Workers must put on gloves and masks to avoid inhaling the dust or contaminating the product. Production lines get checked for bacteria, heavy metals, and mold. Food laws and pharmacopoeia rules govern everything from manufacturing temperature to trace allergen residues. Pharmaceutical-grade glucose faces tighter specs compared to the type poured into soda, but identical principles guide both—purity, safety, and reliable supply chains.
Where Glucose Leaves Its Mark
Few people realize how deep glucose runs. Bakers swear by it for keeping bread moist, confectioners rely on it to avoid sticky messes, hospitals drip it into IV bags, and sports drinks cranks it up for cyclists and marathoners. In the lab, glucose solutions make feeding cell cultures look easy. Even pet food and beauty products benefit from glucose’s humectant properties, keeping things supple and palatable. Fuel for fermentation bioreactors and a staple in diagnostic kits, glucose props up industries from brewing to biotech.
Digging for New Answers: Glucose in Research
Medical researchers use glucose metabolism as a window into diabetes, obesity, and cancer. Tracking radioactive glucose lets doctors spot tumors faster than ever. In environmental science, scientists watch how fast bacteria chew through glucose to gauge pollution clean-up progress. Plant scientists—people I’ve worked with—track glucose flows when measuring drought stress or genetic tweaks. Its scientific worth shows no sign of declining; ongoing studies explore enzyme improvements, better crop strains, and smarter delivery in pharmaceuticals.
Toxicity Research: What the Data Shows
Glucose on its own does not poison in the way lead, cyanide, or most artificial additives do. The worry spins around dose: consume in excess and type 2 diabetes, obesity, and heart disease numbers climb. Early animal studies confirm that overdose leads to insulin resistance, while human cases link massive exposure to metabolic injury. Researchers debate at what level glucose tips from lifeline to risk. Fact remains—too much of anything carries a price. For kids with metabolic disorders like glycogen storage disease, even a shortage spells trouble. The challenge isn’t glucose, it’s balance.
The Path Ahead for Glucose
Farmers and industry insiders see changing winds. Rising skepticism about sugar’s health effects has shifted consumer demand from refined sugars to plant-based syrups and alternative sweeteners. Some labs push for starch-free glucose via engineered yeast or algae, skipping the cornfields altogether to spread risk and lower environmental footprints. Pharmaceutical research targets “smart” glucoses—modified for slower or more controlled release—or combined with insulin analogs for next-level treatments. One field—regenerative medicine—bets on glucose-based gels to grow tissues and organs outside the body. The oldest sugar may gain a new reputation, as biochemistry keeps finding ways to tweak, tune, and refine what looks from the outside like the world’s most basic carbohydrate.
What is Glucose used for?
A Fuel Our Cells Appreciate
Glucose plays a starring role in keeping us alive and kicking. This simple sugar gets a bad rap sometimes, but it’s what our body’s engine craves to run strong. Eat bread, potatoes, or even fruit, and glucose enters our bloodstream, ready to get to work. Our brains in particular hunger for steady supplies—thinking and remembering suffer without it. Anyone who’s felt foggy after skipping meals knows what I mean. The body’s demand doesn’t quit, and that’s why missing out on carbohydrates often leads to that unmistakable drag.
Powering Medical Emergencies
Hospitals stash glucose for a good reason. For folks with diabetes, a quick fix comes in the form of glucose tablets or gel when blood sugar plummets. I’ve seen a friend of mine suddenly go pale and shaky after a workout, saved only by a sugary drink nearby. Medical teams use intravenous glucose in emergencies when someone can't eat yet needs an energy boost fast, like after surgery or during infections. This approach brings people back from the edge.
A Must-Have in Sports and Endurance
Endurance athletes don’t wait for their tanks to run dry. Sports gels, drinks, and candies supply a shot of glucose mid-race to help push through the wall. I’ve tried running longer distances without fueling, and feet start feeling heavy once muscle stores dip low. Sprinkle in the right sweet snack, and suddenly a long ride or hike starts to feel doable again. Professional teams treat glucose as something more than just a pick-me-up: it’s often part of a carefully planned strategy.
Chemistry Beyond Nutrition
Food and medicine take up a chunk of glucose’s day job, but manufacturers use it, too. Factories break it down into syrups for soft drinks, baked goods, and candies. In the lab, glucose turns into vitamin C, citric acid, or even biodegradable plastics. Many of the sweet foods in a store have roots in corn, wheat, or potatoes—processed down until the end result is pure glucose or a close cousin.
A Closer Look at Health and Glucose
Blood sugar levels swing too high or too low for millions of people, especially with type 1 and 2 diabetes. Letting things get out of balance leads to nerve pain, vision loss, and kidney problems. Monitoring keeps things safer. Health experts talk about the dangers of empty calories, but it’s not glucose to blame—it’s eating far more than the body burns off. In truth, a steady supply of glucose supports muscle repair, immune function, and energy to play with kids or head out for a hike.
Keeping It in Check
Finding that sweet spot depends on choosing whole grains, fruits, and vegetables over sugar-laden sodas and desserts. Cooking at home and reading food labels put power in our hands. Some circles push low-carb diets, but personally, they always leave me sluggish. Learning how our bodies act after a meal—a bite of fruit in the afternoon, oatmeal for breakfast—helps us make practical choices almost every day.
Looking Ahead
Research explores ways to make better use of glucose in treating metabolic diseases, sports performance, and managing hospital care. Tools that track blood sugar in real time already help millions make on-the-fly changes. The focus on simple actions, like eating balanced meals and staying active, brings old-fashioned wisdom back into the spotlight. Glucose remains essential, but smart choices keep it working for—not against—us.
Are there any side effects of taking Glucose?
Why People Reach for Glucose
Glucose grabs attention fast. Sugar energy can sound like an easy fix when feeling drained, dealing with a dizzy spell, or facing a long run. In most emergency rooms, doctors slip a glucose drip into the arm of someone who passes out from low blood sugar. Diabetics may chew a tablet or gulp a sweet drink when numbers drop too low. For athletes, glucose gels line up in gym bags and trail running vests. No secret—glucose brings energy, keeps our cells running, and feels like a lifeline to many.
The Risks of Popping Too Much Glucose
Not many folks talk about the downsides of taking glucose without thinking things through. Eating a little sugar now and then, or treating hypoglycemia as instructed, doesn’t usually spell trouble. A different story surfaces with frequent or heavy use, and that’s the one I learned the hard way after experimenting with energy gels for long bike rides.
I noticed headaches, stomach pains, and a jittery sort of tiredness once the burst faded away. Turns out, research lines up with what I felt. Taking in extra glucose pushes blood sugar up fast. For most healthy people, the body handles this spike, but problems creep in for those with diabetes, prediabetes, or anyone who might be insulin resistant. Large doses can trigger a rebound crash, setting off more cravings and swings in energy and mood.
Digestive System Takes a Hit
Stomach cramps and bloating are familiar to folks loading up on glucose, especially the liquid kind found in gels or drinks. Glucose draws water into the gut, leading to diarrhea for some—especially in big amounts or on an empty stomach. Athletes sometimes talk about “runners’ gut”, which can stop a race before it even starts.
Not just athletes feel the stomach squeeze. Kids given glucose at the hospital for illness often refuse the next dose after a sour belly or nausea kicks in. Even a healthy adult can face similar symptoms after overdoing sugary treats during a stressful week.
Heart and Metabolic Red Flags
Repeated glucose spikes set the stage for bigger health problems. The Harvard School of Public Health links added sugar, like glucose, to higher heart disease risk. The rapid jump in blood sugar increases pressure for the pancreas to release insulin, and over time, the system can burn out. That paves the way for type 2 diabetes, unhealthy cholesterol, and fatty liver disease. I’ve seen family members struggle to manage their diet, and it’s tough to watch those habits catch up later in life.
Drinking glucose drinks each day, or even several times a week, may not sound dangerous in the moment. The consequences often stack quietly until lab work or a doctor’s warning shines a light. Following the Nutrition Facts label and keeping serving sizes in check saves headaches in the future.
Finding a Safer Approach
Better choices exist for keeping blood sugar steady. Eating whole foods—fruits, whole grains, nuts—slows down how quickly glucose hits the bloodstream. For people dealing with diabetes, checking blood sugar before adding glucose makes a difference. Doctors and dietitians help tailor a plan by looking at the bigger picture and a person’s unique health story.
Glucose works well in the right moment, but treating it like a quick snack or a cure-all brings more problems than solutions. Paying attention to portion size and the way the body responds goes a long way. Knowledge and moderation matter, and anyone with doubts can check with a healthcare professional before relying on glucose fixes or supplements.
How should Glucose be stored?
The Simple Science of Keeping Glucose Safe
Ask anyone working in a lab, pharmacy, or food factory about raw materials, and it only takes a few minutes before storage comes up. Glucose sounds simple—just sugar, right? But the rules change once you leave the kitchen. I’ve seen stacks of bags go bad and sticky messes turn up when nobody paid enough attention to something as basic as keeping out moisture. It's not just about keeping things tidy; bad storage can ruin a whole batch, cost a bundle, or even risk consumer safety.
What Glucose Needs to Stay at Its Best
Glucose soaks up water from the air, and that spells trouble. Clumping, caking, or even microbial growth are regular headaches. People sometimes think clear bags on a shelf are fine. But air with a hint of humidity turns powdery glucose into something better saved for the compost heap. Keeping it dry makes all the difference. A tightly sealed, moisture-proof container stops problems before they start. A good polypropylene drum beats a thin plastic bag every time.
The other enemy is heat. High temperatures speed up any change, including caramel smells or color shifts, especially for glucose syrup. So a cool, shaded storage spot works better than a sunlit windowsill or a corner near the furnace.
Don’t Ignore Cleanliness
Contamination can sneak up quickly. I saw a shipment returned once because evidence of pests turned up in sugar drums. Glucose invites bugs, so storing it close to open bins or with cracked lids doesn't work. A few crumbs or spills give insects a perfect invitation. Some places manage well just by checking for spills, sealing up lids after each use, and keeping the warehouse clean.
Checking Labels Matters
Stress multiplies when a batch of product turns cloudy, doesn’t dissolve, or tastes off, only to learn the glucose sat well past its expiration date or in the wrong container. Labeling every drum and checking dates stops confusion. I always push for a quick check on delivery numbers and conditions—received on a humid day, left in a damp storeroom, and the clock starts ticking.
Where Things Slip Up—and How to Fix Them
Shortcuts come back to bite hard. People sometimes use “temporary” containers, like bags meant for salt or flour, and ignore the warning signs, thinking it’s harmless for a week. But breaking up hardened glucose may seem minor—until you need consistent quality or you’re dealing with health products.
Training makes a big difference. A few times a year, a reminder about proper storage and quick checks brings better results than complicated posters or one-off emails. I’ve worked with teams who took pride in keeping things spotless and sealed, and it was obvious in the finished product.
Some places install simple humidity monitors. These devices cost less than a wasted drum of glucose. If numbers start creeping up, someone investigates before loss hits stock.
Trust and Standards Matter
Following food and pharmaceutical storage standards isn’t just about box-checking. It builds trust. I’ve felt the relief when independent audits came through without a hiccup, all because basic habits stuck: dry, cool, tightly sealed. Insurance companies ask for records. Buyers scan for any hint of spoilage. It’s not overkill—it’s just smart business.
Looking back, careful handling prevents more stress, saves money, and keeps everybody healthier. There’s nothing fancy about good glucose storage, but it rewards attention every single day.
Can diabetics use Glucose products?
Understanding The Basics
Anyone living with diabetes has probably heard warnings about sugar and carbohydrates a hundred times. Glucose, the simplest form of sugar, plays a starring role in the body’s energy process, so its management matters a lot for people with diabetes. The question about using glucose products isn’t just about avoiding sweet treats; it’s about understanding how the body with diabetes reacts to extra glucose, and when it can actually help.
How Glucose Affects The Body
In diabetes, the body's system for moving glucose from the bloodstream into the cells doesn't work as well as it should. This leads to blood sugar levels that spike or dip too easily. For people without diabetes, a gulp of glucose brings a quick blast of energy, and the insulin in their body quickly brings levels back down. With diabetes, the body’s insulin either doesn't show up as needed or doesn’t do its job correctly. This means anything with “glucose” on the label should be approached with knowledge and some caution.
Not All Glucose Products Are Off Limits
Some products, like glucose tablets and gels, have a serious purpose. They are a lifeline during hypoglycemia—when blood sugar collapses below the safe line. Emergency guidelines from trusted diabetes groups always recommend using fast-acting glucose if blood sugar dives too low. Glucose tabs act quickly, are easy to measure, and don’t carry the fat, fiber, or protein that slow down absorption. This isn’t controversial—these products save lives, and plenty of people with diabetes keep them nearby for peace of mind.
Daily Life, Daily Choices
The trouble comes from regular or recreational use of glucose-rich food and drinks. In my own family, I’ve seen how easy it feels to grab a regular soda or candy during a tough moment, but the short relief can spiral into hours of blood sugar swings. Health agencies report that regular extra glucose leads to worse long-term blood sugar trends and higher chances of problems like heart disease and nerve trouble. For people with type 2 diabetes, it usually makes sense to steer clear of added glucose products, unless a doctor gives the green light for specific situations.
The Role Of Education And Self-Monitoring
Trusted information comes from places like the American Diabetes Association and experienced professionals. They all push for “knowing your numbers”—checking blood sugars regularly, and learning what different foods and supplements do to your body. Glucose in pure form has a predictable, fast spike, which is important knowledge. With newer tech like continuous glucose monitors, people can see real-time changes and make smarter choices faster. The tools are out there, but using them well takes time and patient support.
Smart Solutions And Community Support
If you or someone you love has diabetes, it doesn’t mean living in fear of every carbohydrate. It means building routines, making swaps where possible, and learning what rescue products belong in your bag or car. Some folks lean on community—support groups, diabetes educators, online forums—where real-world advice fills in the gaps. Food labels deserve a closer look; not just for “sugar” but for “glucose,” “dextrose,” and short ingredient lists that tell the true story.
Aiming For Balance
Living with diabetes means respecting glucose while not giving up on the enjoyment of food or the peace of normal life. Safe use of glucose products comes down to knowledge, planning, and checking in with a healthcare provider who understands your day-to-day challenges. There’s always more to learn, but small steps, shared experiences, and trusted resources help manage the ups and downs more smoothly.
What is the recommended dosage for Glucose?
Glucose Dosage Relies on Context
Most folks don’t think much about glucose outside of a cup of sweet tea or a bag of Skittles. Under the skin, glucose powers every cell in the body. Doctors and nutritionists often find themselves talking about "recommended dosages," but real life doesn’t hand out one-size-fits-all answers. For a healthy adult, the body works hard to keep blood glucose in a certain range—typically fasting glucose sits between 70 and 100 milligrams per deciliter (mg/dL). After a meal, it’s normal for the number to rise to 140 mg/dL or so. The body’s own insulin does the heavy lifting, shuttling glucose into cells for energy.
Medical Use: Getting Specific
Some situations call for a more measured approach. Take intravenous glucose, for example. In hospitals, doctors give patients a glucose solution for a variety of reasons—from hypoglycemia (low blood sugar) to supporting nutrition in people who can’t eat. Most medical teams follow weight-driven calculations: for adults, a standard rate is 4 to 5 mg/kg/minute for regular metabolic needs. Children and infants process glucose differently, often requiring more frequent monitoring and adjustments. In emergencies, like severe hypoglycemia, the usual “dextrose 50%” (D50W) ampoule gives a 25g dose all at once. That’s not something a person should try at home without guidance—glucose overdosing gets dangerous quickly, potentially leading to spikes that injure organs and scramble electrolytes.
Everyday Life and Diet
Most people meet their daily glucose needs by eating complex carbohydrates, which digest more slowly than straight sugar. Dietary guidelines suggest that carbs make up around 45–65% of daily calories. That translates into 225–325 grams of total carbohydrates for a 2,000-calorie diet, which the body steadily breaks down into glucose. For someone with diabetes, carefully planning when and how much carbohydrate goes into each meal often matters as much as what’s eaten. Tools like carbohydrate counting help avoid dangerous highs and lows. From my own experience living with a diabetic family member, I’ve seen how the process takes thoughtfulness and sometimes quick action.
The Dangers of Too Much—and Too Little
Glucose isn’t something to mess around with, especially without advice from a healthcare professional. Overdosing, even on a regular diet, can come from excess consumption of sweetened drinks or candies, stacking risks for insulin resistance and diabetes. Fluctuations in blood sugar also contribute to feeling tired, cranky, or dizzy. On the flip side, too little glucose stops the brain from functioning at its best. Hospitals track glucose levels for a reason: hypoglycemia can lead quickly to confusion, loss of consciousness, and seizures.
Solutions and Better Habits
Preventing trouble starts with education and steady habits. Knowing how much carbohydrate is found in foods makes it easier to keep things stable. For anyone on medication that affects blood sugar—like insulin or certain pills—regular monitoring and conversations with a doctor stay key. Fitness and a varied diet help the body process sugars more smoothly. Apps and continuous glucose monitors have changed the game for people at risk, allowing trends to be tracked in real-time. Technology gives power back to patients, but no gadget replaces good advice from a trusted provider. Health depends not just on numbers, but on choices made each day, shaped by knowledge and support.
| Names | |
| Preferred IUPAC name | (2R,3S,4R,5R)-2,3,4,5,6-pentahydroxyhexanal |
| Other names |
Dextrose Grape sugar Blood sugar Corn sugar |
| Pronunciation | /ˈɡluːˌkoʊs/ |
| Identifiers | |
| CAS Number | 50-99-7 |
| Beilstein Reference | 1720225 |
| ChEBI | CHEBI:17234 |
| ChEMBL | CHEMBL39573 |
| ChemSpider | 5582 |
| DrugBank | DB00122 |
| ECHA InfoCard | 03be9435-d4c8-49ba-9abb-5074b6c07c98 |
| EC Number | 3.2.1.20 |
| Gmelin Reference | **Gmelin Reference: 83268** |
| KEGG | C00031 |
| MeSH | D005947 |
| PubChem CID | 5793 |
| RTECS number | LC5600006 |
| UNII | I5QVK0URT3 |
| UN number | UN2811 |
| Properties | |
| Chemical formula | C6H12O6 |
| Molar mass | 180.16 g/mol |
| Appearance | White or colorless crystalline powder or granules |
| Odor | Odorless |
| Density | 1.54 g/cm³ |
| Solubility in water | Soluble |
| log P | -3.24 |
| Vapor pressure | 1 mmHg (20°C) |
| Acidity (pKa) | 12.6 |
| Basicity (pKb) | ~28.0 |
| Magnetic susceptibility (χ) | Diamagnetic |
| Refractive index (nD) | 1.465 |
| Viscosity | Thick, syrupy |
| Dipole moment | 1.74 D |
| Thermochemistry | |
| Std molar entropy (S⦵298) | 209.2 J·mol⁻¹·K⁻¹ |
| Std enthalpy of formation (ΔfH⦵298) | -1273 kJ/mol |
| Std enthalpy of combustion (ΔcH⦵298) | -2801 kJ/mol |
| Pharmacology | |
| ATC code | A11GA01 |
| Hazards | |
| Main hazards | Not hazardous under normal conditions of use. |
| GHS labelling | GHS labelling of Glucose: Not classified as hazardous according to GHS; no pictogram, signal word, hazard statement, or precautionary statement required. |
| Pictograms | GHS07 |
| Signal word | Warning |
| Hazard statements | Not a hazardous substance or mixture. |
| Precautionary statements | P264, P270, P301+P312, P501 |
| NFPA 704 (fire diamond) | 1-0-0 |
| Autoignition temperature | 630 °C |
| Lethal dose or concentration | LD50 (rat, oral): 25,800 mg/kg |
| LD50 (median dose) | 25,800 mg/kg (rat, oral) |
| NIOSH | SDZ60 |
| PEL (Permissible) | 15 mg/m³ |
| REL (Recommended) | 70–99 mg/dL |
| IDLH (Immediate danger) | No IDLH established |
| Related compounds | |
| Related compounds |
Fructose Galactose Glucose oxidase Cellobiose Sucrose Starch Glucose 6-phosphate Glucuronic acid |