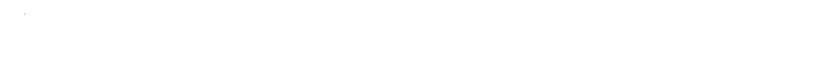Dihydroxypropyltheophylline: History, Properties, and Practical Realities
Historical Development
Back in the mid-twentieth century, researchers spent countless hours in cramped laboratories, working late into the night among the smell of spilled solvents and chalk dust, hunting for new xanthine derivatives with therapeutic promise. Theophylline already had a reputation as a solid bronchial dilator, offering relief for those fighting chronic asthma and obstructive pulmonary disease. Chemists saw the chance to tweak its molecular structure, hoping to build on its strengths and mute its side effects. Dihydroxypropyltheophylline came out of this search; its development reflected equal parts curiosity and practical thinking. Through persistent experimentation with hydroxypropyl substitutions, investigators at several European and American universities brought this compound to life. Their hope: a smoother clinical profile with reliable respiratory benefit. The careful studies and discussions published in the ’70s and ’80s are still worth reading, often written with more candor and humility than today’s polished reviews.
Product Overview
The main draw for dihydroxypropyltheophylline lies in its relationship with theophylline. The two spring from the same chemical family, sharing a backbone but diverging at the side chains. This change means differences not just in how the compound works inside the body, but in how it feels under your hands and smells in a beaker. For the pharmaceutical world, it offers a shot at tailored treatment, something a little gentler for people who struggled with the unpredictable peaks and troughs of pure theophylline. Multiple generic names have sprung up according to local habits, but the scientific community still references its IUPAC name for clarity during international conferences and technical exchanges.
Physical & Chemical Properties
A dish of dihydroxypropyltheophylline shows itself as a white to off-white crystalline solid. Most formulations favor the anhydrous variant, skipping unnecessary moisture. The structure offers a melting point tucked firmly above 200°C—so it survives both the warehouse in summer and the heat of a compounding pharmacy. Its medium-water solubility sits in a practical window, making it more accessible for both oral and injectables than some finicky xanthines. The molecular weight bundles all the expected carbons, hydrogens, nitrogens, and oxygens into a tight figure, allowing relatively straightforward quality control using high-performance liquid chromatography—a practice every good QC lab stands by. Smelling it, old-timers sometimes mention an earthy undertone, not quite coffee, not quite hay, a relic of its xanthine heritage.
Technical Specifications & Labeling
The bottles rolling off the production line ought to carry clear information on purity, moisture percentage, and particle size, with a sharp eye for anything lingering from synthesis—residual solvents or trace metals. Regulators long ago stopped turning a blind eye to anything short of full disclosure. Pharmaceutical standards usually put the minimum purity threshold above 98%. Sophisticated machines scan for even the smallest impurity, not just to satisfy paperwork but to safeguard the folks at the other end—the children, grandparents, workers with dust-choked lungs—who depend on a trouble-free medicine. Effective labeling doesn’t just rush through a checklist; it walks the pharmacist through expiration dates, storage advice, and batch traceability. In more than one workplace, I’ve seen how smart, clear labeling helps people avoid real risk.
Preparation Method
Chemical synthesis of dihydroxypropyltheophylline starts with a routine methylation of xanthine, followed by careful introduction of hydroxypropyl groups. Small-scale chemists favor a stepwise approach, making sure intermediate products reach the right structures before pushing ahead. Commercial plants, armed with bigger reactors and tighter environmental controls, rely on automated monitoring. Heavy use of chromatographic separation helps weed out unwanted isomers and leftover reactants, keeping the process reproducible. Safety protocols matter just as much as reaction yields—extended exposure to strong acids, bases, and certain organic solvents used along the way can spell trouble without real personal protective equipment and ventilation.
Chemical Reactions & Modifications
Dihydroxypropyltheophylline lends itself to more than one kind of modification depending on company goals. Pharmaceutical chemists sometimes attach other functional groups to tweak the duration of action or make it more water-soluble for specific patient needs. On the research bench, few resist the urge to test substitutions at different nitrogen positions on the xanthine ring. These little changes can sometimes alter both metabolism and binding to adenine receptors in unpredictable ways—both a blessing and a curse for development timelines. For any variation moving past the academic stage, stability against oxidation and light becomes a recurring challenge, one that only careful formulation and packaging manages to control.
Synonyms & Product Names
Walk into a hospital in a half dozen different countries, and you’ll likely hear a fleet of names for dihydroxypropyltheophylline. Alongside the IUPAC label, clinicians and pharmacists use several trade names—some crafted by local manufacturers looking to stand out, some handed down from the original patent application. International pharmacopoeias do their best to reconcile the different synonyms, but old habits die hard. Conferences spent sorting out language quirks remind me how communication in medicine relies as much on shared conventions as it does on science. I’ve seen real confusion on the ward when similar xanthine names jostle for attention on patient charts, so accuracy still pays.
Safety & Operational Standards
Manufacturing plants demand respect for dihydroxypropyltheophylline’s potential risks to both personnel and the wider environment. Personal experience tells me never to get comfortable around bulk containers—protective gear only works when it becomes second nature. Management takes its cue from OSHA recommendations and European Chemicals Agency guidance, enforcing regular training sessions on dust suppression, respiratory masks, and safe chemical storage. Handling the compound in a compounding pharmacy calls for close attention to powder dispersion and spill response. Environmental engineers invest in filtering equipment to keep airborne releases well below mandated thresholds. Years of regulatory inspections taught the industry that shortcuts end up costing more than they save—not just in fines, but in trust.
Application Area
Respiratory medicine offered the obvious field for dihydroxypropyltheophylline at the start. Its promise as a smoother-acting bronchodilator struck a chord for patients struggling with asthma, bronchitis, or chronic obstructive pulmonary disease. Over time, clinical curiosity led prescribers to try it in a few other cases—off-label for some mild cardiac arrhythmias, or occasionally as an adjunct in neonatal apnea. In veterinary clinics, it found a home treating certain breeds prone to airway problems. Clinical decision-making continues to weigh its role against newcomers, but the reality on the ground: some patients respond better to this molecule than the more aggressive or costlier alternatives. Real-world patterns show the enduring power of practical experience over glossy marketing.
Research & Development
Basic research digs into the details of pharmacodynamics and metabolism. Academic labs keep pushing to find what makes dihydroxypropyltheophylline tick—some use animal models, others prefer high-throughput receptor-binding assays. The drive to understand absorption, distribution, and metabolic breakdown in different populations keeps a rotating cast of graduate students busy, generating data that eventually filters down into dosing guidelines and side effect warnings. Industry investment leans toward formulation, optimizing delivery for both convenience and patient adherence. Both camps keep an eye on personalized medicine, considering how a person’s genetics might shift the expected response. These days, research collaboration across borders feels more necessary than ever, as regulatory approval grows less forgiving of incomplete answers.
Toxicity Research
Every new drug runs straight into the wall of toxicology; dihydroxypropyltheophylline never got a free pass. In animal studies, researchers documented dose-dependent effects—nausea, tremor, changes in heart rate—echoing what old-school doctors saw with theophylline. Some volunteers, despite their healthy profiles, reacted with unexpected intensity, underlining just how narrow the margin for safety sometimes feels with methylxanthines. Failures and setbacks in toxicity trials still matter: they save future patients from avoidable risk. Modern studies look for long-term impacts on liver and kidney health, and routine blood monitoring guides every cautious prescriber in the community.
Future Prospects
Looking ahead, dihydroxypropyltheophylline faces stiff competition from newer molecules and evolving delivery methods. Genetic research will likely carve out tailored use-cases, letting clinicians select this compound for those with proven metabolic strengths or sensitivities. Environmental pressure on pharmaceutical factories will nudge improvements in waste reduction and greener synthesis. In my years working alongside clinical teams, I’ve learned that old molecules, when re-examined through new technology and open research, can gain a fresh lease on life. People will keep searching for safer, more predictable bronchodilators. Some new combinations or formulations might secure a place for dihydroxypropyltheophylline well into the next generation—provided commitment to both rigorous science and real-world usability remains the rule.
What is Dihydroxypropyltheophylline used for?
Real-World Use in Asthma and COPD
Dihydroxypropyltheophylline, often found on pharmacy shelves as doxofylline, brings a breath of relief to many people struggling with asthma and chronic obstructive pulmonary disease (COPD). These lung conditions make each breath feel like lifting weights. Patients need more than just quick fixes—they rely on treatments that let them take deeper, easier breaths day in and day out.
How It Stands Apart from Other Theophyllines
Doctors have prescribed theophylline for decades, but its side effects can send patients back to the hospital. Palpitations, stomach aches, and upset sleep leave many looking for better choices. Doxofylline tried to tackle those problems. It keeps the beneficial bronchodilator effects but skips some of the heart-racing side effects that have given theophylline a tough reputation. In real clinic visits, this difference matters. People living with asthma want confidence that their medicine won’t trade one struggle for another.
The Evidence Shaping Its Role
Researchers keep close eyes on published studies when a drug promises something new. Large studies in India, Europe, and beyond point to doxofylline as a solid tool to relax airway muscles and reduce flare-ups. Unlike other xanthines, doxofylline avoids the tangled web of interactions with foods and other medications. This simple profile draws gratitude from patients managing several prescriptions at once. A family member once told me how juggling pills can turn daily routines into puzzles. Simpler options mean fewer phone calls to the pharmacy and less worry about food restrictions.
Side Effects and Safety
No medicine counts as perfect. Doxofylline, though milder than its older cousin, sometimes brings headaches, nausea, or mild digestive complaints. Yet compared to classic theophylline, these issues tend to appear less often or with less intensity. This means less concern about hospital stays for toxicity. According to a 2017 meta-analysis in Respiratory Medicine, doxofylline showed a favorable safety profile in adults with COPD. That’s more than just statistic—it’s peace of mind for the person turning to a rescue inhaler in the middle of the night.
What Stands in the Way
Not everyone gets equal access to newer drugs. Some regions still lean on theophylline as the cheaper, more familiar option. Doctors and patients end up making choices based on what’s available, not always what works best. Insurance coverage gaps put doxofylline out of reach for many who could benefit.
Steps Toward Better Treatment
If better options exist, more education remains key. Pulmonologists, pharmacists, and patients all benefit from clear information. I’ve seen family doctors attend workshops, bringing lessons back to small clinics where patients rarely see a specialist. Policy makers and health systems can help by ensuring newer medicines get fair reviews for reimbursement. Pharmaceutical research has already carved out something safer here; now the challenge is making it reachable for every person whose lungs need a break.
What are the possible side effects of Dihydroxypropyltheophylline?
Understanding Dihydroxypropyltheophylline
Most folks haven’t heard of dihydroxypropyltheophylline unless they’ve spent time combing through medical literature or ingredient lists. This compound comes from the theophylline family, a group known for their work in easing breathing troubles, especially in people dealing with asthma or certain lung diseases. The name might sound technical, but the idea isn’t new: medicines in this group help relax muscles in airways and clear out mucus, so breathing gets a bit less labored.
Why Side Effects Matter
Nobody likes unpleasant surprises. Learning about a new medicine, prescription or not, means figuring out the good and the not-so-good. Side effects turn up even with the most trusted medications. Theophylline-based drugs come with stories from patients who felt jittery, found sleep hard to come by, or got hit with stomachaches. Dihydroxypropyltheophylline lives in that same family, bringing benefits but asking a few trade-offs.
Common Side Effects Seen with Theophylline Compounds
Theophylline and its relatives often crank up heart rates. Folks sometimes mention a racing pulse, more noticeable if someone already deals with high blood pressure or irregular heart patterns. Headaches and nausea pop up too, and some report feeling irritable or anxious. Changes in appetite sometimes creep in. Stomach distress can mean cramps or diarrhea—less fun for anyone just trying to breathe easier.
My time working in clinics taught me no two people react the same way. An older patient once described feeling “wired” after a single low dose. The nurse and I reviewed her other meds—turned out her body processed the drug slower, building it up much higher than expected.
Looking Out for Rare but Serious Problems
Most folks will never brush up against the worst-case side effects, but the possibility deserves a good spotlight. Seizures, harsh chest pain, or hammering palpitations rarely sneak in, but stories do exist. The risk spins up if levels get too high—sometimes because the body’s liver can’t clear it fast enough, or if another drug blocks its breakdown.
Lab results back up these claims. A 2022 review published in Pharmacology Research showed more side effects in patients who took too much theophylline or forgot to watch interactions with other drugs like antibiotics or seizure meds. The FDA’s own medication guides highlight these dangers for anyone with liver or kidney troubles.
Practical Advice and Safer Use
Doctors check blood levels with theophylline, and for good reason. Small tweaks in dose lead to big changes in the body. Symptoms—like pounding heartbeats or unexpected vomiting—point to blood levels tipping too high. Pharmacists play an important role, checking for medicines that make side effects worse.
Open communication helps. Anyone starting a new medicine, especially with a long name and a history of tricky side effects, needs straightforward instructions. Simple reminders—take with food if your stomach feels queasy, watch for sleep problems, don’t mix with caffeine—can help sidestep trouble.
Patient education often saves the day. Reminding people to report headaches or digestive problems early means side effects rarely get out of hand. For dihydroxypropyltheophylline, the old lessons from its theophylline cousins still ring true.
How should Dihydroxypropyltheophylline be taken or administered?
Knowing the Substance
Dihydroxypropyltheophylline doesn’t come up in everyday talk, but it sits in the same family as theophylline—a compound used often in respiratory medicine. For people dealing with asthma or chronic obstructive pulmonary disease (COPD), theophylline and its derivatives can make breathing a little easier. The way a person takes these medications can mean the difference between real relief and a world of problems.
Oral Route: Familiar, But Demanding Precision
Some folks get Dihydroxypropyltheophylline as a tablet or capsule. Swallow and wash it down with water. That simple gesture hides a bigger truth: this isn't a pill you can take whenever you have a cough or feel short of breath. The liver chews up these drugs at a pace different in every person. A dose that lets one person breathe easy can give someone else jitters, headaches, or even more dangerous side effects. Forgetting to check blood levels leaves too much to chance.
Doctors sometimes ask for blood tests to keep an eye on the amount moving around in a patient's system. People who like coffee or have certain medical conditions might process the drug faster or slower. That detail matters a lot, especially for something that can play games with both the lungs and the heart.
Mixing With Food and Other Medicines
A glass of milk or a plate of food holds the power to shift what happens with each dose. Some medications mix poorly with Dihydroxypropyltheophylline, raising risks of dangerous spikes or drops. Grapefruit juice comes up a lot in stories about medication mix-ups, and with good reason—a glass in the morning can block certain enzymes, leading to higher levels in the blood.
People who take antibiotics, seizure medications, or even simple antacids should talk with a doctor or pharmacist before starting Dihydroxypropyltheophylline. Taking a new medication without that chat invites trouble, even if things seem fine at first.
The Importance of Timing and Dosage
Anyone with experience in chronic asthma knows the feeling of waiting for relief when breathing gets hard. Dosing Dihydroxypropyltheophylline on a set schedule—never too soon, never skipping—strongly shapes long-term results. Cutting pills or stretching doses can mean trouble. I’ve seen folks land in the emergency room, not realizing a few missed doses might send things downhill quickly.
Alternatives and Personalization
Medicine isn’t one-size-fits-all. Some people respond well to theophylline derivatives, others don't. Inhalers often take center stage in breathing problems because they act fast and stick closer to the lungs. Pills like Dihydroxypropyltheophylline enter the bloodstream and impact more than just the chest. Being open and honest with the doctor—about side effects, missed doses, even eating habits—lets them tailor the plan. Personalized care gives a better shot at living comfortably, not just surviving symptoms.
Practical Steps for Those Taking Dihydroxypropyltheophylline
Anybody starting this medication should keep a written record of doses and symptoms. Set reminders on your phone. Bring up every symptom, even ones that seem small, at your next appointment. Use the same pharmacy each time—a trusted pharmacist can notice problems with renewing prescriptions or answer questions that crop up late at night.
No single answer solves every challenge, but by keeping the conversation going with healthcare providers and staying aware of your own body, it gets easier to safely use Dihydroxypropyltheophylline and keep breathing easy.
Is Dihydroxypropyltheophylline safe for children or pregnant women?
Understanding What We’re Dealing With
Dihydroxypropyltheophylline is a bit of a mouthful—it’s a derivative of theophylline, a drug that has been around in asthma treatment for decades. People rely on theophylline because it opens up the airways and helps with breathing during an asthma attack or in chronic cases. But as soon as you see chemical tweaks like “dihydroxypropyl” added, it gets tricky to judge safety without up-to-date research.
Looking at Current Safety Data
Drug safety matters the most for kids and during pregnancy. Their bodies process chemicals differently. Theophylline has well-documented risks. It can cause nausea, headache, heart palpitations, and worse if the dose runs high. Too much can even prompt seizures or irregular heartbeat. For anyone, that’s serious—but in a child or fetus, consequences run higher. During my pharmacy years, we watched theophylline levels closely for this reason.
I’ve checked the largest medical databases and safety guidance. Dihydroxypropyltheophylline isn’t found in pediatric or pregnancy guidelines from reliable sources such as the FDA, AAP, or WHO. Absence of strong safety data spells a big red flag, especially compared to more established asthma medications. Regulators like the FDA require extensive testing before approving a drug for kids or pregnant women, because their bodies don’t just scale down from adult doses. Drug metabolism shifts because of age, size, pregnancy hormones, and other factors.
What Doctors and Pharmacists Say
Doctors hesitate to prescribe anything outside the gold-standard medicines, especially for groups at high risk. Pediatricians and obstetricians stick to drugs with a proven record because mistakes can’t be reversed. My old colleagues discuss this often: lack of long-term safety research on new or rare medications should steer us toward caution. In real life, I’ve watched parents scouring the internet looking for answers when doctors suggest switching medications for their kids. Their worry is real and justified.
What Matters for Families
Parents and soon-to-be moms want clear answers, not chemical jargon. People just want to know: “Will this help and not cause harm?” With dihydroxypropyltheophylline, science can’t provide a sure answer yet. I’ve seen families turn to online forums, but these rarely separate scaremongering from science. Too often, promising-sounding treatments don’t stand up to long-term studies.
Trust grows from history and results. Albuterol, inhaled steroids, and old-theophylline have long safety records. If dihydroxypropyltheophylline ever appears in a doctor’s prescription pad, it has to bring evidence, not just hope.
Taking Action
If you’re facing an asthma diagnosis or breathing problem with a child or during pregnancy, ask questions. Don’t settle for guesswork. Request safety data and alternatives. Ask your provider to break down risks and reasons for every medication. If new drugs lack strong clinical evidence in these sensitive groups, stick to medicines with established safety.
Families shouldn’t play guessing games with health. Anyone offering new treatments owes clear proof of both benefit and safety—not just in headlines, but in published studies and data your doctor can trust.
Can Dihydroxypropyltheophylline interact with other medications?
Mixing Medications Isn’t Just a Guessing Game
Every time I watch someone pull out a bag of pills from their cabinet, I remember how easy it is to overlook how medications bump into each other inside the body. Dihydroxypropyltheophylline sits in this crowded space, especially for people using it for respiratory support or other off-label reasons. It seems harmless enough — a cousin of the theophylline family — yet, like most drugs, it walks the same tightrope: It can help, but it can also get tangled up with other medications and tip the balance.
How Dihydroxypropyltheophylline Moves in the Body
A big part of how any drug interacts with others comes down to enzymes, particularly those in the liver like CYP1A2. Theophylline and related compounds, including dihydroxypropyltheophylline, often use these enzymes to break down. If something slows these enzymes down — say, antibiotics like ciprofloxacin or fluvoxamine (an antidepressant) — the breakdown doesn’t happen as quickly. Drug levels shoot up, and side effects barge in. Faster breakdown, on the other hand, happens with smokers or with seizure medicines like carbamazepine, leaving less of the drug to do its work.
Common Pills That Bump Heads with Dihydroxypropyltheophylline
With heart medications, blood pressure drugs, and antibiotics, dihydroxypropyltheophylline often finds itself in crowded company. Some fats and cholesterol drugs (like statins) don’t like to mix with it either, risking higher toxicity. Even herbal supplements can stir the pot. St. John’s Wort, for example, speeds up enzyme action, which might cut down how much dihydroxypropyltheophylline sticks around. On the flip side, caffeine — hiding in coffee or over-the-counter pain pills — acts a lot like theophylline, so their effects just stack up.
Real-Life Effects Don’t Always Seem Obvious
People tend to expect a dramatic reaction if medicines clash, but it’s often slow and sneaky. Headaches, stomach trouble, shaky hands, or even skipped heartbeats can creep in with little warning. It doesn’t always take a big dose — sometimes it’s a small daily shift. That’s what happened to someone I know who balanced a daily asthma med and antibiotics; before long, jitteriness and a pounding heart became unwelcome guests. Adjustments had to be made, and it was a clear reminder that invisible interactions can spark real trouble.
Watching Out and Making Smart Choices
Doctors and pharmacists map out prescriptions for a reason. They pull up medical records, cross-check for clash points, and adjust doses with each new prescription. If you add supplements, over-the-counter meds, or even a new kind of vitamin, the balance can shift. Open conversations and full lists of medications can mean the difference between smooth sailing and a rough patch at the doctor’s office.
What Helps Keep Families Safe
Tracking all medicines, noting every supplement, and sharing the list at checkups keeps the lines clear. Apps and pill organizers help too, but the real power comes from treating health care like it’s a team sport. It’s worth asking about new symptoms and reporting changes, even if they seem small. Information helps professionals prevent medication traffic jams that lead to side effects or less effective treatment. By taking the time to ask and inform, anyone can lower the risk of unwanted interactions, especially with compounds like dihydroxypropyltheophylline.
| Names | |
| Preferred IUPAC name | 3-(2,3-Dihydroxypropyl)-1,3-dimethyl-7H-purine-2,6-dione |
| Other names |
Diproxophylline Dihydroxypropyltheophylline 3,7-dihydro-1,3-dimethyl-1H-purine-2,6-dione 7-(2,3-dihydroxypropyl)theophylline |
| Pronunciation | /daɪˌhaɪdrɒksiˌproʊpɪlˌθiːəˈfɪliːn/ |
| Identifiers | |
| CAS Number | 1476-68-4 |
| Beilstein Reference | 695127 |
| ChEBI | CHEBI:49575 |
| ChEMBL | CHEMBL2106656 |
| ChemSpider | 5516 |
| DrugBank | DB08997 |
| ECHA InfoCard | 38e22260-bacd-4d8d-98b1-7fa2b57258fc |
| EC Number | 3.2.2.17 |
| Gmelin Reference | 112137 |
| KEGG | C07762 |
| MeSH | D018245 |
| PubChem CID | 65484 |
| RTECS number | YU9625000 |
| UNII | Y3H4402622 |
| UN number | UN3077 |
| CompTox Dashboard (EPA) | DTXSID60153403 |
| Properties | |
| Chemical formula | C10H14N4O4 |
| Molar mass | 240.23 g/mol |
| Appearance | White crystalline powder |
| Odor | Odorless |
| Density | 1.3 g/cm³ |
| Solubility in water | soluble |
| log P | -0.6 |
| Vapor pressure | 0.000102 mmHg at 25°C |
| Acidity (pKa) | 8.60 |
| Basicity (pKb) | 1.89 |
| Magnetic susceptibility (χ) | -78.9×10⁻⁶ cm³/mol |
| Refractive index (nD) | 1.530 |
| Viscosity | Clear, colorless liquid |
| Dipole moment | 4.44 D |
| Thermochemistry | |
| Std molar entropy (S⦵298) | 180.7 J·mol⁻¹·K⁻¹ |
| Std enthalpy of formation (ΔfH⦵298) | −1096.9 kJ/mol |
| Std enthalpy of combustion (ΔcH⦵298) | -3225 kJ/mol |
| Pharmacology | |
| ATC code | R03DA08 |
| Hazards | |
| Main hazards | Harmful if swallowed. Causes serious eye irritation. Causes skin irritation. |
| GHS labelling | GHS07, Exclamation mark |
| Signal word | Warning |
| Hazard statements | H315: Causes skin irritation. H319: Causes serious eye irritation. H335: May cause respiratory irritation. |
| Precautionary statements | Keep container tightly closed. Store in a cool, dry place. Avoid contact with eyes, skin, and clothing. Wash thoroughly after handling. Use with adequate ventilation. |
| NFPA 704 (fire diamond) | 1-1-0 |
| Flash point | 143°C |
| Lethal dose or concentration | LD₅₀ (oral, rat): 695 mg/kg |
| LD50 (median dose) | LD50 (median dose): 732 mg/kg (rat, oral) |
| NIOSH | DB13779 |
| PEL (Permissible) | Not established |
| REL (Recommended) | 0.63 |
| Related compounds | |
| Related compounds |
Theophylline Acefylline Etofylline |