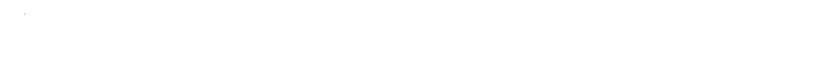Methyldopa Hydrate: A Deep Dive into Its Past, Present, and Future
Historical Development
Today, Methyldopa Hydrate plays a steady role in healthcare, but its history dates back to the early wave of antihypertensive therapies. In the 1960s, doctors faced a real lack of effective oral medications for controlling high blood pressure. Methyldopa offered a new path by targeting the central nervous system to help control blood pressure, offering an alternative to older medications known for harsh side effects and limited success. The shift Methyldopa brought mattered; it improved treatment for pregnant women and patients who struggled with the more aggressive options. Early research and clinical experience solidified its reputation, especially for obstetricians managing preeclampsia. This isn’t a relic of the past; Methyldopa is still included on the World Health Organization’s List of Essential Medicines, a testament to the value it delivers decades after it first gained approval.
Product Overview
Methyldopa Hydrate belongs to the class of centrally acting antihypertensive agents. By converting to alpha-methylnorepinephrine in the brain, it dampens signals that tighten blood vessels, leading to decreased blood pressure. Available mostly as oral tablets but also manufactured for injection, this product supports physicians working with obstetric hypertension, chronic hypertension, and hypertension unresponsive to standard regimens. With other medication options ballooning over recent years, Methyldopa stands resilient due to a special combination of efficacy for certain populations and a solid safety profile, especially for those who need gentle management. Its continued manufacture under various brands signals lasting clinical faith in its value.
Physical & Chemical Properties
A solid grasp of Methyldopa Hydrate begins with its appearance: white or almost white crystalline powder. Water solubility ranks moderate, which can prove useful for both oral and injectable formulations. Chemically, Methyldopa Hydrate carries the formula C10H13NO4·H2O and a molecular weight around 229.23 g/mol. Odorless, stable under dry conditions, and with a melting point near 300°C, this substance does not degrade quickly at room temperature. Its amphoteric nature allows it to react with both acids and bases, which shapes how it handles in pharmaceutical processing. Knowing the hands-on characteristics—its stability, water affinity, and melting behavior—helps chemists and pharmacists maintain consistency batch-to-batch.
Technical Specifications & Labeling
Pharmaceutical standards for Methyldopa Hydrate remain demanding. Purity levels reach above 98%, and finished products come with labels specifying exact dosing, storage instructions, and identification of its hydrate state. USP, EP, JP monographs guide the essential testing for impurities and active content. Packaging information lists the hydrate status, which matters for compounding and dosing precision. Labeling captures warnings about abrupt withdrawal, interactions with MAO inhibitors, and suitability in pregnancy. Each of these requirements grows from decades of safety data, adapting with regulatory advances to protect those who rely on exact dosages to stay healthy.
Preparation Method
Production of Methyldopa Hydrate typically starts with 3,4-dihydroxyphenylacetaldehyde as the base. Chemists introduce alpha-methylation steps under carefully controlled temperature and pH, followed by the addition of ammonia or its salts. The reaction transforms early intermediates to Methyldopa, and water is used to crystallize it into its hydrate form. Purification through recrystallization and filtration strips away unreacted compounds, leaving behind pure Methyldopa Hydrate. This careful synthetic path, tuned over decades, is critical for meeting pharmaceutical standards and avoiding residual contaminants that could affect efficacy or safety in patients.
Chemical Reactions & Modifications
Methyldopa Hydrate’s chemical backbone lets it face a few modifications in research, such as forming esters or conjugates for targeted delivery. In practical use, it resists oxidation under normal storage, but reacts strongly to strong acids or oxidizers. Under lab conditions, researchers sometimes modify the carboxylic acid group or alter the amine for experimental compounds. These reactions often reveal minor changes to its pharmacology, yielding insight into drug design for next-generation antihypertensives. Most industrial producers, though, stick closely to the original synthesis, guarding patient safety and consistent pharmacological action.
Synonyms & Product Names
Methyldopa Hydrate appears on pharmacy shelves and laboratory inventories under a host of names. Commercially, Aldomet stands out as the most widely recognized brand, though generic labels abound. Other names include Alfa-Methyldopa, L-Methyldopa, and the less common Aldoril (in combination products). For regulatory and research documentation, synonyms such as 3-Hydroxy-α-methyl-L-tyrosine and Methyldopanum reflect its chemical heritage. Brand proliferation has made it easier for health systems and clinics worldwide to ensure availability, even as specific suppliers change over time.
Safety & Operational Standards
Years of experience in the field have shaped robust rules for handling Methyldopa Hydrate. Medical staff receive training on its specific side effects: drowsiness, dry mouth, and sometimes, a drop in blood cell counts. In manufacturing settings, technicians use gloves and eye protection to prevent skin or mucous membrane contact, conscious of its gentle but real irritant properties. Pharmacies and labs follow the established handling and disposal protocols, as leftover material enters hazardous waste streams designed to protect the environment. Good Manufacturing Practice (GMP) regulations, which guide every clinical batch, come from decades of learning how small impurities or process missteps can hurt patient trust and outcomes. Safety around pregnant patients, especially, receives close attention due to its place as a frontline therapy.
Application Area
Methyldopa Hydrate takes on a core role for patients dealing with chronic high blood pressure, especially those who fall into special categories. Pregnant individuals struggling with preeclampsia benefit from its proven track record—it lowers blood pressure without harming fetal health, something no other antihypertensive matches quite as reliably. Physicians also lean on it for patients who can’t tolerate newer, more expensive options. Its action inside the central nervous system results in effective, gentle lowering of blood pressure, with few dangerous interactions. Countries with limited drug access keep Methyldopa in wide circulation because of its affordability and compatibility with resource-strapped health systems.
Research & Development
Research labs revisit Methyldopa Hydrate, focusing on optimizing its synthesis for environmental aims or pursuing new derivatives that might carry even fewer side effects. Clinical research tracks post-marketing safety across populations, especially as generics expand in developing countries. Investigators have explored how Methyldopa impacts immune activity or neuroprotection, branching out from strict blood pressure management. This kind of work helps maintain its relevance, uncovering new clinical niches even as newer medications come to market. Collaborations between chemists and clinicians push incremental improvements in purity or drug delivery, keeping Methyldopa at the center of cost-effective hypertension control.
Toxicity Research
Methyldopa Hydrate’s long-term use in real-world settings generates vast safety data. Most patients tolerate it well, though fatigue and mild liver enzyme elevations occur. Regular monitoring in high-risk groups helps sort rare but serious risks—hemolytic anemia, hepatotoxicity, and psychiatric effects. Toxicologists study these pathways in animal models to spot potential warning signs before clinical problems arise. Due to its metabolism through catechol pathways, researchers watch for subtle impacts on neurotransmitters, providing robust data for package labeling and prescriber education. After so many years, the clear safety profile seen in pregnancy and chronic care solidifies Methyldopa’s reputation, but continuing toxicology research dials in recommendations for each new patient population.
Future Prospects
Methyldopa Hydrate doesn’t fade into history books just yet. Its fortitude in healthcare grows from consistent safety, reliability for expectant mothers, and steady cost. As drug-resistant hypertension surges, clinicians sometimes return to older therapies, rediscovering what works without cutting-edge price tags. Chemists experiment with new salt forms or delivery technologies, striving for fewer side effects and easier administration. In low-resource hospitals, Methyldopa’s endurance brings critical stability to hypertension care. Broader research into its neuroprotective aspects might unlock paths not yet traveled. As industry and healthcare systems juggle scarce resources and patient diversity, Methyldopa offers a reminder that valuable therapies thrive when they balance decades of experience, safety, and accessibility.
What is Methyldopa Hydrate used for?
What Is Methyldopa Hydrate?
Methyldopa hydrate shows up in many medical conversations about managing blood pressure. It owes its reputation to the treatment of high blood pressure, especially for people facing either sensitive health situations or unique conditions. Doctors often pick it for pregnant women battling preeclampsia because it offers a good safety profile compared with many other options. Not every drug works for everyone, and not every medicine plays well with pregnancy. This one, though, shows up in treatment guidelines again and again.
Tackling High Blood Pressure in Pregnancy
Many people learn about their high blood pressure during pregnancy. For families expecting a baby, news like this brings fear and stress. I have had relatives stare down those hospital walls while worrying about the health of a child not yet born. Methyldopa acts as a lifeline for those parents. It helps lower blood pressure without bringing in too much risk to the developing fetus. Many other antihypertensive medicines create unwanted side effects during pregnancy or show the potential for birth defects, so methyldopa still holds its place in clinical practice long after its introduction back in the 1960s.
How It Works
Methyldopa enters the nervous system and interrupts the messaging that tightens blood vessels. By tricking the brain, it helps blood flow through more relaxed vessels, resulting in lower blood pressure. Some folks report feeling tired when using it because it slows those nerve signals. For some, especially older patients, that drowsiness becomes a roadblock in daily life.
Side Effects and Cautions
No medication acts in isolation. Methyldopa brings a list of possible side effects. Besides tiredness, some people face headaches, dry mouth, or swelling. In rare cases, the liver reacts strongly, which means doctors run occasional blood tests to watch for signs of trouble. I have seen patients worry about these side effects, wondering if better options exist. For people not pregnant or not able to tolerate methyldopa, other drugs enter the conversation, but each comes with its baggage.
Why Its Use Still Matters
Despite newer medications with slicker marketing, methyldopa still comes up in clinics and hospitals. Some countries keep it on their essential medicine lists for a reason—safe use in pregnancy and a long track record back up its place on the shelf. It does not fix every blood pressure story, and many never touch it, but those in high-risk pregnancies know it offers one of the safest ways to take control.
Looking Forward
Managing blood pressure often becomes a dance of trial and error. Open conversations with doctors, letting them know about side effects, help keep care on the right path. Services making blood pressure checks easier and regular follow-ups can catch problems faster. Research keeps rolling out fresh alternatives, but no fancy new medicine can replace real listening between patient and doctor. That's the best bet for safer care and healthier outcomes, whether it's methyldopa or something new.
What are the common side effects of Methyldopa Hydrate?
Understanding Methyldopa Hydrate
Methyldopa hydrate has a big part in managing high blood pressure, especially for folks dealing with hypertension during pregnancy. Decades of research place it on the list of trusted medications. Still, as with any effective medicine, it brings a series of side effects worth knowing before getting started.
Fatigue and Drowsiness: More Than Just Feeling Tired
Most people who try methyldopa notice the fatigue first. It hits harder than a bad night's sleep. I've seen friends nod off in the afternoon, blaming the medicine, and their doctors confirming the link. This sedation comes from methyldopa’s impact on the brain’s regulatory centers, calming nerves to drop blood pressure. Some patients might need to adjust schedules—napping or taking breaks at work becomes part of daily life. According to studies, close to half of patients can expect this tiredness at some level.
Impact on Mood and Mental Focus
Occasional mood swings or brain fog can appear, turning simple tasks into struggles. Concentration drops, conversations get fuzzy, and daily routines might slip. Anxiety or even mild depression might creep in. While only a minority face these issues, keeping loved ones, coworkers, or care teams in the loop makes a real difference. Doctors often monitor these changes because early detection helps decide if the dose needs a tweak—or if the medication needs a switch.
Headaches and Dizziness
A sudden wave of dizziness can catch folks off guard, especially standing up too fast. Methyldopa drops blood pressure, and the brain sometimes lags in adjusting. Some patients get mild headaches that linger through the day. Simple fixes—hydration, rising slowly, frequent snacks—help manage symptoms. But severe spells, or blackouts, need a prompt call to a doctor. The CDC and Mayo Clinic both warn of this risk and recommend patients keep count of these episodes.
Digestive System Upsets
Nausea or mild stomach upset shows up on the list of common side effects. Constipation can turn chronic if someone isn’t careful with fiber and water intake. These symptoms tend to ease as the body adapts, but staying in touch with a physician matters if stomach problems persist or hunger disappears. Doctors sometimes suggest starting methyldopa with food.
Effects on the Liver and Blood
Regular blood work often becomes part of the routine, though patients rarely look forward to it. Methyldopa can lead to changes in liver enzymes or, rarely, a reduction in red blood cells—a condition called hemolytic anemia. From clinical practice and from advice given by established sources like UpToDate, these usually only pop up after months of use. Prompt testing every few months helps catch problems early so doctors can decide if stopping the medication is right.
Managing or Preventing Side Effects
Staying ahead of these symptoms sometimes calls for lifestyle tweaks. Drinking enough water, eating regular meals, and resting during the day can all help. Building a solid relationship with a healthcare team allows side effects to be addressed before they threaten daily life. Open conversations, honest reporting of new or worsening symptoms, and routine check-ups form the support network that keeps high blood pressure controlled without letting side effects take over.
More Resources and Reliable Support
Always check with healthcare professionals about medication questions. Accurate sources—from the American Heart Association to the FDA—keep information reliable and current. Patients benefit from knowledge backed by science, real-world experience, and a partnership mindset between patients and doctors.
How should Methyldopa Hydrate be taken or administered?
Methyldopa Hydrate: The Why Behind Each Pill
Methyldopa hydrate shows up in the daily life of anyone dealing with high blood pressure, especially for pregnant women. This medication’s long-standing history in hypertension therapy says something about its value. Too many people underestimate routine when it comes to blood pressure pills, but the reality is simple: every skipped dose means the risk for a heart problem quietly climbs. Blood pressure often comes with no warning signs, so keeping a steady habit really does make a difference.
Taking It at the Right Time Counts
Some folks treat pill time as a suggestion rather than a rule. Still, research out of the British Journal of Clinical Pharmacology underlines that taking methyldopa hydrate at the same time daily helps keep blood pressure steady. I remember watching my own father, who often forgot his morning dose and ended up with headaches and dizziness. There’s no substitute for a visible pillbox, set alarms, or a daily routine—these small actions give structure to a treatment that protects vital organs.
Food or No Food: Is There a Difference?
Doctors do suggest this medicine gets taken with or without food. For many, a small snack helps ease any stomach troubles. I’ve seen that a cracker and a glass of water came to my grandmother’s rescue more than once, helping her avoid that queasy feeling. Drinking a full glass of water never hurts, either—it helps the medicine do its job without sticking in your throat.
The Dose Isn’t the Same for Everyone
This drug doesn’t come in a one-size-fits-all plan. A qualified provider takes health history, age, and any other medication into account before settling on the right amount. People with kidney or liver disease may need close monitoring or adjusted amounts due to methyldopa’s effect on those organs. No internet chart offers shortcuts here. Every dosage question needs a face-to-face or a telehealth consult.
Mixing Alcohol or Other Medications Leads to Trouble
Alcohol sometimes looks harmless, but mixing it with blood pressure medication can turn an evening drink into a dizzy, dangerous mess. Some folks believe in doubling up on blood pressure pills if they miss one, but doubling the dose piles on risks instead of solutions. Communication with the prescriber is always better than guessing games. Even basic over-the-counter medicines or supplements can change methyldopa’s effects. Taking time to check with a pharmacist saves a lot of hassle, and sometimes even a hospital trip.
Side Effects and What to Watch For
Fatigue, dry mouth, or mild swelling might show up early on for some people. It helps to track symptoms in a notebook, as patterns are easier for doctors to spot and adjust accordingly. Rarely, someone might notice yellowing skin or fever—these deserve quick medical attention. No one should feel shy about reporting side effects; those honest updates help fine-tune the balance between blood pressure control and daily quality of life.
What Keeps This Process Safe
Routine lab checks cover liver function and blood counts. Test reminders taped to the fridge work wonders. Trust builds when the patient and provider stay open about what’s working (and what isn’t). Keeping up regular appointments, asking questions, and sticking to one pharmacy streamlines care, especially if prescriptions change.
Simple Solutions for Everyday Use
A plastic pillbox, a dependable schedule, and a little patience go a long way. Incorporating methyldopa hydrate into a consistent part of the morning or evening routine supports a healthier heart in the long run. Staying mindful of side effects and keeping honest communication with healthcare professionals shields against many of the pitfalls that can crop up. The path may not always be smooth, but small, steady steps matter most.
Are there any contraindications or precautions with Methyldopa Hydrate?
Methyldopa Hydrate: Who Should Be Careful?
Methyldopa Hydrate helps control high blood pressure. Doctors often choose it for pregnant people, since it has a good track record for safety during pregnancy. Still, this medicine comes with some important warnings. Overlooking these can mean serious trouble for certain patients.
Liver Problems: A Hidden Threat
If you have a history of liver disease, or if you’ve ever had hepatitis caused by drugs, methyldopa is not a good idea. It can restart old liver issues, and sometimes it causes hepatitis even in people who never had problems before. Drug-induced hepatitis is no small thing—it can turn severe, with symptoms like yellowing skin and eyes, fever, and aches.
That personal experience of watching a relative struggle through medication-triggered hepatitis stays with me. The confusion—why a pill that lowers blood pressure could leave someone too tired to get out of bed—underscores why doctors want to check liver function before starting, and a few weeks into treatment. Regular monitoring is not just paperwork. It can be the difference between catching liver stress early and a full-blown crisis.
Blood Disorders: Anemia and More
Methyldopa can lower red blood cell counts and cause hemolytic anemia. Symptoms like tiredness, shortness of breath or dark urine can sneak up, so it’s wise to take them seriously. In my volunteer work at health fairs, I’ve seen folks whose unexplained fatigue turned out to be anemia, but they chalked it up to stress. This drug sometimes drops healthy blood cell levels without warning. Routine blood work lets care teams catch problems before they spiral.
People who already have anemia, or any other issue that impacts their blood, should talk to their doctor before using methyldopa. Often, those with autoimmune conditions like lupus or a history of blood cell issues will need another blood pressure medicine.
Mental and Physical Side Effects
Feeling severely down or confused? Methyldopa sometimes brings on depression, nightmares, or muddled thinking. I’ve heard people describe “brain fog” and unexplained sadness after starting certain blood pressure drugs. With methyldopa, doctors weigh these risks, especially if you live alone or have a history of mood changes. Seizures are another rare, but serious, reaction.
Kidney Issues and Other Concerns
Patients with kidney disease find methyldopa can make things worse. Because the drug leaves the body through the kidneys, existing kidney damage means the medicine can build up to dangerous levels. Dosing adjustments—sometimes even frequent lab checks—become crucial for folks with reduced kidney function. The same goes for anyone on dialysis.
Even if methyldopa has worked in the past, skin reactions or unexplained fever signal trouble. Both could be early warnings of bigger problems to come. If you break out rashy or notice swelling in your face, stop the medicine and call a doctor.
How to Stay Safe: Some Steps Forward
The script is simple: honest conversations, regular check-ups, and listening to the body. Pharmacists and doctors can help spot the warning signs if patients keep them in the loop. Wearing a medical ID and making sure family knows your medicine list helps, too. For new prescriptions, it pays to keep track of changes in mood, energy, or skin. Caught early, most problems can be fixed before they do lasting harm. If methyldopa isn’t the right fit, there are always other options on the table.
Can Methyldopa Hydrate be used during pregnancy or breastfeeding?
What Expectant Parents Face with High Blood Pressure
Up in the OB-GYN clinic, pregnant patients with high blood pressure often hear the name “methyldopa.” The diagnosis brings anxiety, not just about their own health but about whether anything taken will affect the child. For years, doctors have turned to methyldopa for women battling hypertension while pregnant.
Decades of use speak to its reputation. The World Health Organization and major women’s health groups rank it as a preferred choice, mainly for its record of not causing damage to the fetus. I’ve seen many mothers walk in with blood pressure surging beyond safe levels—risking preeclampsia or stroke. Methyldopa, in most cases, has brought those numbers down without triggering concerns on the fetal ultrasound.
Why Doctors Choose Methyldopa in Pregnancy
The medicine works by relaxing blood vessels and slowing the heart slightly. Unlike many other antihypertensives, methyldopa rarely causes birth defects. Large studies dating back to the 1970s and 1980s looked at thousands of pregnancies. These reviews ran the numbers: no spike in miscarriage, no jump in birth defects, and no unusual child development problems after birth. Methyldopa didn’t make problems, it helped solve them.
Doctors still don’t hand it out like candy. My own training hammered home that every drug during pregnancy gets scrutinized. The team weighs risks and benefits. If a pregnant woman’s blood pressure tips too high and diet or gentle exercise won’t budge the numbers, methyldopa often takes the stage.
Possible Side Effects and Tradeoffs
No pill skips side effects. People on methyldopa sometimes feel tired, dry mouthed, or slightly low on energy. Some get headaches or constipation. These side effects make some patients want to quit. I tell people it’s not about suffering through but about telling a doctor how they feel. Sometimes a switch in medicine works; sometimes the benefits outweigh the nuisance.
Rare reports mention liver problems. Most clinics run a simple blood test before starting, then recheck while on the drug. This looks out for anyone facing trouble early.
What About Breastfeeding?
After delivery, the next question pops up fast: will methyldopa slip into breastmilk and hurt the baby? Tiny amounts do enter milk. Research teams have measured the levels—almost always low. Pediatricians reviewing the evidence agree: no record of harm, no pattern of babies reacting badly.
That said, breastfeeding parents get reminders to watch for unusual tiredness or trouble feeding. If anything seems off, they bring it up with their medical team right away.
Keeping Mothers and Babies Safe
Blood pressure in pregnancy isn’t something to ignore. Along with methyldopa, doctors sometimes prescribe alternatives like labetalol or nifedipine. No single option fits everyone. Medication choices happen after talking through history and test results.
That’s why smart, open conversation matters. If someone feels uneasy, sharing those feelings helps guide safer care and gives space to talk about alternatives or more support. For families facing high blood pressure, methyldopa remains a key option—tested by time, still under the watchful eye of researchers and health professionals.
| Names | |
| Preferred IUPAC name | (2S)-2-amino-3-(3,4-dihydroxyphenyl)-2-methylpropanoic acid monohydrate |
| Other names |
Aldomet Methyldopate L-α-Methyldopa α-Methyldopa Methyldopar Hydroxy-alphamethyldopa |
| Pronunciation | /ˌmɛθ.ɪlˈdoʊ.pə ˈhaɪ.dreɪt/ |
| Identifiers | |
| CAS Number | 41372-08-1 |
| Beilstein Reference | 1108728 |
| ChEBI | CHEBI:44186 |
| ChEMBL | CHEMBL1139 |
| ChemSpider | 15415 |
| DrugBank | DB00968 |
| ECHA InfoCard | EU0000095-1 |
| EC Number | 253-056-0 |
| Gmelin Reference | 62735 |
| KEGG | D08229 |
| MeSH | D008756 |
| PubChem CID | 441285 |
| RTECS number | OM8225000 |
| UNII | L3V0468Z1G |
| UN number | “UN2811” |
| Properties | |
| Chemical formula | C10H13NO4·H2O |
| Molar mass | 238.241 g/mol |
| Appearance | white to almost white crystalline powder |
| Odor | Odorless |
| Density | 1.2 g/cm3 |
| Solubility in water | Soluble in water |
| log P | -2.11 |
| Vapor pressure | <0.01 mm Hg (20°C) |
| Acidity (pKa) | 2.72 |
| Basicity (pKb) | 8.89 |
| Magnetic susceptibility (χ) | -92.5×10^-6 cm³/mol |
| Dipole moment | 6.1 D |
| Thermochemistry | |
| Std molar entropy (S⦵298) | 165.7 J·mol⁻¹·K⁻¹ |
| Std enthalpy of formation (ΔfH⦵298) | -932.5 kJ/mol |
| Pharmacology | |
| ATC code | C02AB01 |
| Hazards | |
| Main hazards | Harmful if swallowed. May cause damage to organs through prolonged or repeated exposure. Causes serious eye irritation. Causes skin irritation. |
| GHS labelling | GHS05, GHS07 |
| Pictograms | GHS07,GHS08 |
| Signal word | Warning |
| Hazard statements | H302: Harmful if swallowed. |
| Precautionary statements | P264, P270, P301+P312, P330, P501 |
| NFPA 704 (fire diamond) | 2-2-0 |
| Flash point | 126°C |
| Lethal dose or concentration | LD50 oral rat 4,370 mg/kg |
| LD50 (median dose) | LD50 (median dose) = 3700 mg/kg (oral, rat) |
| NIOSH | MU0893000 |
| PEL (Permissible) | 10 mg/m³ |
| REL (Recommended) | 0.5~2 g daily |
| Related compounds | |
| Related compounds |
Methyldopa Levodopa Carbidopa Dopamine Alpha-methyldopamine |