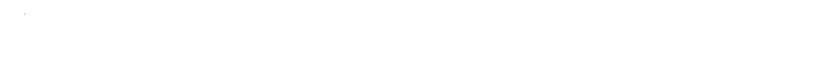L-Thyroxine: Tracing the Journey and Shaping the Future
Historical Development
L-Thyroxine tells a story that weaves together curiosity, observation, and biochemical discovery through generations. The first hints about the connection between the thyroid gland and metabolism came from clinicians in the nineteenth century who noticed that removing the thyroid led to a slow decline in both physical and mental vigor. This led researchers down a path where, after decades of trial and error, they finally isolated thyroxine in the early 20th century. Ernst Baumann and E. C. Kendall made huge strides in this space, extracting and identifying the hormone from animal thyroid glands. Synthetic production picked up steam in the 1920s, but mass production didn’t truly take hold until after World War II. By the time doctors began routinely treating hypothyroidism with synthetic L-Thyroxine, the pharmaceutical world had already started searching for more reliable, stable, and scalable production methods.
Product Overview
L-Thyroxine, often known simply as levothyroxine, shows up in many medicine cabinets as a thyroid hormone replacement. Chemically, it mirrors the thyroxine produced naturally in the thyroid, making it a linchpin for restoring proper function when the gland falls short. The pure, crystalline form emerges as either a sodium or free acid salt, but doctors almost always prescribe the sodium salt thanks to its stability. Pills, capsules, and even intravenous forms work their way onto pharmacy shelves, ensuring people with hypothyroidism don’t have to live in a fog of fatigue or weight gain.
Physical & Chemical Properties
L-Thyroxine tips the scales at about 776 g/mol when measured as the sodium salt. Visually, it looks like a fine, white to off-white crystalline powder, with barely a trace of smell or color. The compound dissolves poorly in water, which poses a challenge in tablet formulation, but manufacturers often overcome this by using various excipients. With a melting point around 230°C, this synthetic hormone stands up well against heat during the tableting process. Its structure carries two iodinated aromatic rings—this feature holds the key to its physiological effects. Given its charged, bulky nature, careful handling and formulation steps shape how effectively it gets absorbed and how reliably it delivers consistent blood levels.
Technical Specifications & Labeling
Product labeling for L-Thyroxine carries a clinical weight. Every microgram counts, so tablet and ampoule strengths are precisely listed, typically ranging from 25 to 200 micrograms per dose. Labels highlight the sodium salt content and provide clear directions on storage, usually recommending a cool, dark, dry place to maintain stability. Each batch undergoes analysis for identity, potency, and purity, ensuring results within strict pharmacopoeial limits—most commonly, U.S. Pharmacopeia (USP) or European Pharmacopoeia (Ph. Eur.) standards. Companies must warn of cross-contamination with traces of animal proteins, gluten, or lactose, a critical consideration for individuals with sensitivities or allergies.
Preparation Method
Creating L-Thyroxine starts in a laboratory equipped to handle precision and complexity. Chemists often rely on multi-step organic syntheses beginning with precursors like tyrosine. The process features selective iodination—adding iodine atoms to specific locations on the molecule. Protective groups shield vulnerable sites from unwanted reactions, while solvents and reagents coax the right bonds to form. Purification steps strip away byproducts, and the finished hormone crystallizes out before packaging. This meticulous procedure allows for consistent production without needing animal-sourced thyroid, a shift that lessens the risk of impurities or prions, and supports growing demand.
Chemical Reactions & Modifications
L-Thyroxine's chemistry centers on its four iodine atoms and the ether bond linking two aromatic rings. Aside from the basic synthetic route, researchers have explored modifications like altering the iodine pattern or substituting side chains to craft analogs. Pharmacologists have experimented with deiodinization, creating triiodothyronine (T3). These chemical tweaks offer pathways to both improved medications and deeper biochemical understanding. Such structural changes sometimes unlock faster absorption, altered receptor affinity, or reduced side effects, showing how small modifications influence the final product’s medical potential.
Synonyms & Product Names
Doctors and patients can find L-Thyroxine listed under a host of generic and brand names. Levothyroxine, L-3,5,3',5'-tetraiodothyronine, and LT4 all point to the same molecule. Pharmacies carry it under names like Synthroid, Euthyrox, Levoxyl, Eltroxin, and Euthyrox. This naming spread reflects both regulatory requirements and competitive branding across the pharmaceutical world, but in the end, each acts as a beacon for one shared purpose: restoring healthy thyroid hormone levels.
Safety & Operational Standards
Risk management in the production and handling of L-Thyroxine runs on strict adherence to safety standards. The facility’s air handling, cleanliness, and personal protective measures all play a part in preventing occupational exposure and contamination. Operators receive safety training regarding both the active ingredient and excipient risks, especially as inadvertent inhalation or ingestion can bring about thyroid symptoms. Pharmacies and manufacturers alike document every step to provide clear evidence for regulators and quality auditors. These measures also extend to patient education, with pharmacists supporting therapy adherence, reviewing interactions, and tackling common side effects like palpitations, nervousness, or allergic reactions.
Application Area
The main stage for L-Thyroxine remains hypothyroidism, a condition that can sap vitality and disrupt daily life. Endocrinologists and family doctors alike prescribe it for underactive thyroid, including cases after thyroidectomy, radiation, or autoimmune damage. Some protocols extend its use to manage certain types of goiter, congenital hypothyroidism, or to suppress thyroid cancer recurrence by dialing down thyroid stimulating hormone (TSH) levels. Veterinarians also tap into its benefits for treating similar thyroid conditions in cats and dogs. Its widespread use shapes both the pace and the quality of life for millions, making its reliable supply and quality no small matter.
Research & Development
Ongoing research on L-Thyroxine looks to smooth out rough patches in therapy. Scientists are digging into the molecular genetics of thyroid hormone receptors, seeking to personalize dosing through pharmacogenomics. Drug delivery studies chase down alternative administration routes and formulations to tackle variable absorption or timing challenges. Fixed-dose combinations with triiodothyronine (T3) see scrutiny as researchers hope to mirror natural hormone release more accurately. Clinical studies continue to watch for subtle impacts on bone health, cognition, and cardiovascular health, shaping future refinements and recommendations.
Toxicity Research
Toxicity studies on L-Thyroxine underline its narrow therapeutic window. Overdoses, intentional or accidental, can spark symptoms of thyrotoxicosis: anxiety, rapid heartbeat, weight loss, sweating, and even arrhythmias or seizures in severe cases. Toxicology teams use both animal models and human case reports to track dose-related side effects and risks. Regular blood testing, especially in pregnant women, children, and elderly patients, guides therapy to prevent both under- and overshooting hormone targets. Researchers aim to understand how chronic slight overdosing might nudge long-term risks like osteoporosis or heart disease.
Future Prospects
Looking forward, breakthroughs in precision medicine promise to reshape how L-Thyroxine reaches the individual patient. Advances in genetic screening could allow clinicians to fine-tune dosage based on metabolism type or tissue sensitivity. Long-acting formulations, smart pill technologies, or implantable delivery systems could move past the need for daily medication, tackling the burden of missed doses. Researchers keep probing the hormone’s nontraditional uses, from mood disorders to weight management and even as adjuncts in fertility treatments. The central importance of its quality, stability, and patient support won’t fade as demand for these proven therapies spans the globe. The next era for this venerable therapy will rely on partnership among chemists, clinicians, and patients to keep refining the art and science of thyroid health.
What is L-Thyroxine used for?
The Basics of L-Thyroxine
L-Thyroxine, often recognized by the brand name Synthroid, serves a single, clear purpose in medicine: supporting people whose thyroid glands don’t produce enough hormone. The thyroid sits at the base of the neck, and its job involves more than folks often realize. Without enough thyroid hormone, energy levels dip, weight shifts, and even the heart can act up. My own brother discovered he had hypothyroidism after months of unexplained fatigue and brain fog. Only then did his doctor introduce him to L-Thyroxine, and within weeks, the difference in his mood and stamina stood out to everyone who knew him.
Why the Body Depends on Thyroid Hormone
Think of thyroid hormone as the body’s main temperature regulator. It keeps heart rate steady, helps the brain stay focused, and makes sure food gets turned into energy properly. Without enough thyroid hormone, every system works harder just to get through the day. Research shows untreated hypothyroidism increases the risk of heart problems and slows down many everyday processes. For children, low levels of thyroid hormone mean slow growth and slower mental development, so doctors don’t waste time in starting kids who need it on medication.
Who Takes L-Thyroxine and Why It Matters
Most prescriptions go to people with hypothyroidism—usually caused by Hashimoto’s thyroiditis, a disease where the body turns against its own thyroid. Others start L-Thyroxine after surgery or radiation that removes or damages thyroid tissue. Even after thyroid cancer treatment, a person can’t just “do without” the hormone, making this daily pill essential for life. Pregnant women with thyroid troubles also rely on L-Thyroxine because a mother’s thyroid levels shape her baby’s brain development even before birth. Data from the American Thyroid Association points out that around 12% of the U.S. population will deal with a thyroid problem at some point, so this isn’t a rare issue.
Finding the Right Dose: A Balancing Act
Getting the dose just right takes patience. Blood tests every couple months in the beginning help dial in the amount each person needs. Too little, and symptoms stick around. Too much, and there’s a risk for bone thinning, anxiety, or heart rhythm issues. My friend, a longtime nurse, always reminds her patients not to tinker with the dose themselves. Skipping pills or doubling up can throw the body off in ways you feel for days. A steady routine—taking medicine at the same time each day, away from calcium or iron pills—makes a real difference.
Access and Affordability
One positive is that L-Thyroxine stands as both widely available and affordable, showing up on generic drug lists at most pharmacies. This lowers barriers to proper care, especially for people managing chronic conditions on fixed incomes. Still, doctors stress the value of staying connected to care, not ignoring routine follow-ups, and reporting new symptoms early. Too many patients drop off as symptoms ease, only to come back years later with heart or memory problems tied to skipped medicine.
Looking Ahead at Thyroid Care
Thyroid issues rarely come with flashing warning signs. For many, L-Thyroxine means the difference between dragging through the day and living fully. Regular checkups, understanding the signs when things shift, and focusing on whole-body wellness—nutrition, sleep, exercise—all help make sure L-Thyroxine does its job. For anyone wondering about constant tiredness or stubborn weight changes, checking in with a doctor opens the right conversation and, sometimes, delivers the small pill that brings energy and clarity back to life.
How should I take L-Thyroxine?
Why the Right Routine Matters
L-Thyroxine is more than just a daily pill—it's a lifeline for people who rely on it to keep their thyroid levels in check. I’ve learned from personal experience and listening to medical professionals that skipping doses or taking it haphazardly really throws things off. Thyroid hormones run practically every cell in the body. A little inconsistency, and you’ll feel it in your mood, your energy, possibly even your heart rate. So paying attention to how and when you take this medicine makes a world of difference.
Timing Really Does Make a Difference
I used to pop my L-Thyroxine right after breakfast. Sometimes I even took it with my coffee. My endocrinologist quickly corrected me. He explained how food and certain drinks can block absorption. Studies highlight that taking L-Thyroxine on an empty stomach, ideally at least 30 to 60 minutes before eating, allows your body to use more of the hormone. Dairy, fiber, soy, and iron supplements can all tangle up absorption. So you end up taking more medication for less effect, or chasing symptoms you thought were managed.
Consistency Brings Results
Inconsistent routines lead to lab swings. Blood tests might show wild variations in thyroid-stimulating hormone (TSH), making your doctor chase numbers instead of stability. Once I settled into a habit—same time every morning, nothing but water—I stopped seeing those swings in my results. My doctor had fewer adjustments to make. My mornings became automatic, which was one less thing to think about. Everything else followed: steadier energy, clearer thinking, better living.
Other Medications and Foods Can Get in the Way
I learned the hard way about other pills interfering. Calcium and iron tablets, multivitamins, even antacids mess with L-Thyroxine absorption. So if you take those, give your thyroid pill a good four-hour head start. My pharmacist gave this advice based on published research, not just friendly tips.
Don’t Adjust the Dose Without Asking Your Doctor
It’s easy to think a missed pill or an off day means taking an extra one helps. That’s a big mistake. Overdosing can cause palpitations, anxiety, even bone loss long-term. Underdosing drags you down and brings symptoms back. Doctors use regular blood checks to find your dose, because stress, illness, and age all impact your hormone needs. Self-tweaking turns small issues into big ones fast.
Simple Steps to Make Life Easier
Most people I know who stay consistent keep their pills by the nightstand with a glass of water. They build it into their wake-up routine. Some set a daily phone alarm. Traveling or changing schedules? Keep a few pills in a travel container, so you’re never caught off-guard. Little acts like these build the habit and deliver much better results.
The Big Picture
L-Thyroxine keeps lives running smoothly, but only if respected. Building simple habits—empty stomach, same time, water only, spacing out supplements—works far better than hoping for the best. If symptoms come back or you hit a rough patch, don’t go it alone. Good communication with your healthcare team, backed by blood tests, puts you in the best spot for good, steady thyroid health. It’s not just medication. It’s daily self-care that shows up in everything you do.
What are the possible side effects of L-Thyroxine?
What Happens In Real Life
A lot of people end up taking L-Thyroxine at some point, thanks to underactive thyroid. Doctors prescribe it every day, aiming to help with fatigue, weight gain, and feeling cold all the time. Folks often expect this tiny pill to work miracles overnight. If anyone’s spent months fighting brain fog or low energy, this hope rings true. The thing is, every medication brings its own bag of surprises. L-Thyroxine might do its job, but it’s not all smooth sailing for everyone.
The Jitters: Palpitations and Anxiety
Taking L-Thyroxine can speed up the body in a way that wakes up more than just the sluggish thyroid. Some patients deal with a racing heart, jittery hands, or a wave of anxiety. The science behind it is simple. Too much thyroid hormone acts like a traffic cop waving cars through green lights, fast and nonstop. More adrenaline kicks in, heart rate shoots up, and it’s hard to relax. These side effects usually mean the dosage is too high. Telling your doctor about these feelings makes a big difference. Dosage tweaks bring relief for most.
Sleep Troubles and Sweating
Sleepless nights show up on the list of problems, too. It feels strange to fight fatigue from hypothyroidism, then, after starting L-Thyroxine, find yourself restless at 2 a.m. This happens because metabolism gets a boost, and the body struggles to settle down. Sweating more than usual also pops up—a bit like the body’s thermostat gets stuck. These reactions sometimes fade as the body gets used to the medication. Paying attention to timing can help; taking the pill in the morning fits better with the body’s typical rhythm.
Feelings That Don’t Change Fast Enough
For some, L-Thyroxine doesn’t bring instant relief. Months pass, but symptoms stick around. It’s easy to give up or wonder if the pill works at all. But changing thyroid hormone levels takes patience. Blood tests help track progress. Doctors look at thyroid stimulating hormone (TSH) and free T4 to see what’s happening inside. Adjusting dose based on these results makes the difference. Patience pays off, so does keeping the conversation open with a health care provider.
Bones and Hearts: Long-Term Considerations
Over time, too much L-Thyroxine can push bones to lose strength. Research links high thyroid levels with a greater risk of osteoporosis, especially for postmenopausal women. This doesn’t happen overnight, but it’s worth thinking about. Keeping an eye on bone health, especially after many years of thyroid medication, matters. Heart rhythm issues sometimes come up, too, mostly in older adults whose hearts already work hard. Sorting out the safest dose protects both bones and heart.
Handling the Ups and Downs
Regular communication with a trusted doctor stands as the best solution. Noticing new symptoms and getting blood work helps dial in the finest dose. It isn’t about hitting a magic number—it's about feeling better every day. Supporting thyroid health takes time, and no one has to figure it out alone. Science proves that closely monitored therapy keeps most people safe. Honest feedback at appointments changes lives for the better. L-Thyroxine isn’t perfect, but it turns things around for many when given the right attention.
Can I take L-Thyroxine with other medications?
L-Thyroxine: Why Timing Matters
L-Thyroxine, better known as levothyroxine, makes a real difference for people with thyroid problems. After my own diagnosis of hypothyroidism, I learned this medication isn’t a simple “take it and forget it” pill. L-Thyroxine absorbs best on an empty stomach, and even a cup of coffee can shake up how well it works. Skipping this advice led to some pretty unwelcome lab results for me, so I started taking it first thing in the morning, waiting half an hour before breakfast. The science behind this practice comes straight from studies showing food—especially calcium or fiber-rich meals—blocks the drug from getting fully absorbed.
Mixing Medications: What Gets in the Way?
Plenty of folks need more than just L-Thyroxine each day. Blood pressure drugs, diabetes meds, heart pills, and supplements like calcium or iron can end up in a daily pillbox. Each of these can interact with levothyroxine. For example, antacids, certain cholesterol drugs, and iron tablets all bind to L-Thyroxine, dragging down how much gets into your bloodstream. Even something that seems harmless like a multivitamin can cause problems.
My endocrinologist explained that some common heart medications—like amiodarone or beta blockers—not only push down thyroid hormone levels but also mess with how well thyroid medicine does its job. That’s not something most general practitioners discuss until symptoms show up down the road. As many as one in three people experience a drug interaction with L-Thyroxine over time, leading to fatigue, weight changes, or mood shifts that don’t seem to add up until a doctor spots the culprit.
Real-World Solutions
I see a lot of confusion in online forums and support groups about juggling multiple prescriptions. Just spacing L-Thyroxine apart from other pills can fix most problems. I set a daily alarm: L-Thyroxine goes down with a glass of water at dawn, and nothing else touches my stomach for about 30 minutes. Calcium and iron? They wait at least four hours. Pharmacies now print these reminders right on the bottle labels, but it helps to write the timing down or talk it through with a pharmacist. Doctors know to run thyroid labs a few months after adding new medications, just to catch any shifting levels before trouble starts. Tracking symptoms and sharing changes with your care team adds an extra layer of safety.
Information Quality and Trust
Misinformation floats around, especially on social media. The FDA and major medical groups like the American Thyroid Association consistently remind patients that mixing L-Thyroxine with other medications can leave thyroid disease out of control. Clinical trials back up these warnings. If you ever spot conflicting advice, take it to a pharmacist or an endocrinologist. Trust comes from having the right information and a healthcare team willing to check your whole prescription list every few months. In a world full of distractions, putting medication safety first isn’t complicated, but it requires keeping tabs on the details and staying honest about what you put in your body each morning.
What should I do if I miss a dose of L-Thyroxine?
L-Thyroxine Isn’t Just Another Pill
For anyone with thyroid issues, skipping a dose of L-Thyroxine can trigger anxiety. Thyroid hormones drive how you feel, think, and move throughout the day. Tiredness, mood dips, and “brain fog” often creep in when the hormones drop, turning everyday tasks into small mountains.
The Problem With Skipping a Dose
Missed doses happen. I used to fill a pill organizer every Sunday night, yet I’d still find myself staring at the case one Thursday afternoon, thinking, “Did I take it?” The trouble isn’t the skipped dose itself—missing a single pill usually doesn’t overhaul your hormone levels overnight. Thyroid hormones change slowly. Patience matters, not panic.
What You Should Do
If you remember later on the same day, take the missed dose as soon as you remember. One thing I picked up from my endocrinologist: what you eat and drink can mess with absorption. L-Thyroxine wants an empty stomach—no coffee, no breakfast—just water, then wait a good half hour. If your memory strikes only after lunch, skip the missed dose and pick up where you left off the next day. Doubling up the next morning won’t help and could backfire.
Keeping Hormones Steady
Every body’s a little different. Some folks swear missing a single tablet makes them drag for days, while others barely notice. That comes down to hormone storage—L-Thyroxine hangs around in the body, and levels rise and fall pretty gradually. Still, missing doses regularly makes the thyroid conk out, and over time, your body starts talking back with symptoms. I’ve worked with enough patients who thought their fatigue and weight shifts had other root causes, only to find pill burials in couch cushions.
The Value in Routines and Reminders
Modern life isn’t kind to routines. Work, family, and sleep seem to run on different time zones. What helped me and folks I’ve spoken with is tying the dose to a daily anchor: setting a phone alarm, taping a sticky note to the kettle, tucking the bottle by the toothbrush. Digital pillboxes help, but a simple habit works just as well. The idea isn’t to chase perfection but to aim for consistency. Steady dosing keeps hormone swings out of your way, so you get your days back.
Talk With Your Doctor, Not Just the Internet
Medical advice often gets diluted or dramatized online. If missed doses pile up, or you notice sluggishness, rapid weight changes, or heart palpitations, don’t play guessing games. Check in with your doctor. Blood tests may point to the real problem, which could mean tweaking your dose. L-Thyroxine therapy isn’t one-size-fits-all; doctors adjust based on symptoms, labs, and sometimes even life changes, like pregnancy or new medication.
The Bottom Line
Missing a single dose rarely causes disaster, but making it a habit chips away at your well-being. Building a personal reminder system, sticking with routines, and getting regular thyroid checks let you get the full benefit of treatment. Thyroid health shapes so much of what we feel and do: keeping it on track means less worry and more energy for life.
| Names | |
| Preferred IUPAC name | (2S)-2-amino-3-[4-(4-hydroxy-3,5-diiodophenoxy)-3,5-diiodophenyl]propanoic acid |
| Other names |
Eltroxin Levoxyl Synthroid Euthyrox Levothroid Tirosint Unithroid |
| Pronunciation | /ɛl θaɪˈrɒksɪn/ |
| Identifiers | |
| CAS Number | 51-48-9 |
| Beilstein Reference | 1209335 |
| ChEBI | CHEBI:30696 |
| ChEMBL | CHEMBL1135 |
| ChemSpider | 5461 |
| DrugBank | DB00451 |
| ECHA InfoCard | 100.007.727 |
| EC Number | 3.1.3.56 |
| Gmelin Reference | 17853 |
| KEGG | D08102 |
| MeSH | D013950 |
| PubChem CID | 5819 |
| RTECS number | OJ6955800 |
| UNII | 06LU7C9H1V |
| UN number | UN3249 |
| Properties | |
| Chemical formula | C15H11I4NO4 |
| Molar mass | 776.87 g/mol |
| Appearance | White, round, flat tablets with a score line on one side. |
| Odor | Odorless |
| Density | 1.33 g/cm3 |
| Solubility in water | Very slightly soluble in water |
| log P | -0.4 |
| Vapor pressure | Negligible |
| Acidity (pKa) | 0.13 |
| Basicity (pKb) | 4.26 |
| Magnetic susceptibility (χ) | -65.6×10⁻⁶ cm³/mol |
| Dipole moment | 3.3734 D |
| Thermochemistry | |
| Std molar entropy (S⦵298) | 215 J·mol⁻¹·K⁻¹ |
| Std enthalpy of formation (ΔfH⦵298) | -415.0 kJ/mol |
| Std enthalpy of combustion (ΔcH⦵298) | -8089 kJ/mol |
| Pharmacology | |
| ATC code | H03AA01 |
| Hazards | |
| Main hazards | May cause thyroid hyperactivity, palpitations, anxiety, weight loss, and osteoporosis with overuse. |
| GHS labelling | GHS07, GHS08 |
| Pictograms | take on empty stomach", "take with water", "do not chew |
| Signal word | Warning |
| Hazard statements | Hazard statements: No significant hazards or specific hazard statements are associated with this product. |
| Precautionary statements | Keep out of reach of children. Use only as directed by a physician. Do not use in patients with uncorrected adrenal insufficiency. Store in a cool, dry place, away from light and moisture. |
| NFPA 704 (fire diamond) | 1-0-0-W |
| Autoignition temperature | > 250°C |
| Lethal dose or concentration | LD50 oral rat: 100 mg/kg |
| LD50 (median dose) | LD50 (median dose): Oral-rat LD50: 100 mg/kg |
| PEL (Permissible) | 100 µg/m³ |
| REL (Recommended) | 50–200 micrograms daily |
| Related compounds | |
| Related compounds |
Tetraiodothyroacetic acid Tiratricol Diiodothyronine Triiodothyronine (T3) Thyroid hormone Reverse T3 |