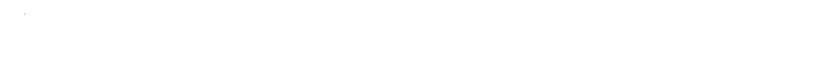Ketoprofen: More than an Anti-Inflammatory Pill
Historical Development
The story of Ketoprofen began in the 1960s. French chemists from Rhône-Poulenc explored several new arylpropionic acids, setting the groundwork for safer anti-inflammatory options. Key research from this period highlighted how aryl substitutes on a propionic acid backbone blocked pathways responsible for pain and inflammation. By the 1970s, after clinical trials swept through Europe, physicians gained another tool to fight joint pain and swelling. Ketoprofen landed on pharmacy shelves worldwide by the mid-1980s, right as people began asking for new alternatives to aspirin and phenylbutazone. Medical adoption grew as more patients, especially those with arthritis, found real relief in a pill that didn’t batter their stomachs quite as harshly as older drugs.
Product Overview
Doctors and pharmacists know Ketoprofen as a nonsteroidal anti-inflammatory drug (NSAID) with a focus on knocking down pain and swelling. It’s easily recognizable in oral capsules, topical gels, patches, and even injectable forms, offering flexibility based on how severe the pain or inflammation gets. Because it blocks both COX-1 and COX-2 enzymes, patients report strong relief from headaches, backaches, and the everyday aches of life. Most health professionals consider it for both short stints of pain and the long haul of chronic conditions. For direct guidance, the product leaflets don’t pad words—Ketoprofen fights pain, it targets inflammation, and its side effect profile, while serious in some, stands well-documented and manageable.
Physical & Chemical Properties
Pure Ketoprofen appears as white or off-white crystals, free-flowing, and moderately dense. What someone sees in a pharmacy capsule is a dry powder that dissolves best in alcohols and common lab solvents, but hardly at all in plain water. Under the microscope, its molecules shape into a racemic mixture—each containing a mirror-image isomer, yet both contribute to the drug’s effect. Melting points hover around 94-97°C, and a unique acidic snap in its structure—courtesy of the benzoyl group and the propionic acid—gives it the punch to disrupt prostaglandin synthesis.
Technical Specifications & Labeling
Packaged Ketoprofen products always state concentration up front, with most oral capsules set at 25mg, 50mg, or 75mg, and topical gels typically echoing a 2.5% or 5% concentration. Labeling requirements run strict, laying out indications, dose, contraindications, plus every flagged risk from GI ulcers to kidney trouble. Whether someone fills a prescription for tablets or grabs an over-the-counter gel, the packaging guidance follows international regulations to ensure patients and providers see the data before any pill gets swallowed or gel rubbed in. Shelf stability ranges several years if kept dry, in a cool place, and away from bright light. In hospital stockrooms, the standardized packaging means there’s little guesswork when tending to patients by bedside or through a home visit.
Preparation Method
Production usually starts with Friedel-Crafts acylation, followed by Grignard reactions and controlled hydrolyses. Chemists build the benzoylpropionic acid nucleus stepwise, always monitoring yields to keep wastage low. Medicinal manufacturers scale up the process by choosing solvents and catalysts that avoid toxic byproducts, aiming for high purity. Purification, often through crystallization and washing, eliminates nearly all trace reactants. The process creates a stable, easily handled powder ready for blending with starches or binding agents in tablets, or dispersal into gels hailed for fast skin absorption. Consistency through tight batch controls matters, and this remains a quiet but critical achievement in any plant making Ketoprofen.
Chemical Reactions & Modifications
Once basic Ketoprofen production wraps up, chemists can create derivatives or improve solubility for topical applications. Esterification and salt formation bring greater absorption, turned into sodium or lysine salts for easier delivery in injectables or oral formulations. Some research labs dive deeper, trying to attach the Ketoprofen molecule to polymers, looking to tailor the drug for slow-release patches or enhanced skin penetration. With the science reviewed in journals, these modifications sometimes unlock patent extensions or lead to lower rates of gastrointestinal side effects through more targeted tissue delivery—a testament to the molecule’s flexibility under a skilled hand.
Synonyms & Product Names
Beyond chemical shorthand like 2-(3-benzoylphenyl)propionic acid, pharmacy clients often meet Ketoprofen under banners like Orudis, Oruvail, Fastum, and Ketoflam. Different countries have local labels, yet the active ingredient inside remains indistinguishable in quality. Papers in medical literature may use synonyms such as Profenid, Biprofen, or Bi-Profenid, all referring back to the same trusted anti-inflammatory core. No matter which name reads on the box, reputable sourcing keeps the patient’s experience similar from one continent to another.
Safety & Operational Standards
Pharmacies and hospitals adopt safety measures for Ketoprofen as they do for any NSAID—clear documentation for allergic patients, watchful dosing for people with compromised kidneys or past GI bleeds, and guidance on quick action at the first sign of rash or swelling. Regulatory agencies demand regular batch testing, environment monitoring in production plants, and annual reviews of adverse events. Technicians who handle raw Ketoprofen powders wear gloves, dust masks, and lab coats, especially during mixing or encapsulation. In disposal, the chemical’s stability pushes facilities toward incineration or certified chemical waste routes. Everyday users benefit from direct instructions on timing with food, staying hydrated, and spotting rare but serious side effects before they spiral out of control.
Application Area
Ketoprofen earns its keep in medicine cabinets and clinics. Doctors reach for it to calm arthritis flares, treat sports injuries, boost post-surgical comfort, and check bad toothaches. Athletes and active people keep gels handy for muscle aches, while veterinarians treat joint pain in horses and dogs with injectable solutions. Small clinical trials have reminded the world about Ketoprofen’s place in managing migraine, menstrual cramps, and even some rare disorders tied to chronic inflammation. Every time a new indication surfaces, it represents another vote of confidence that the compound balances strong medicine with manageable risk—if prescribers and patients work together.
Research & Development
Teams in pharmaceutical labs track how Ketoprofen stacks up against next-generation painkillers, including COX-2 selective drugs and biologic agents. Preparation for new delivery forms, like microencapsulated beads or smart skin patches, combines material science with clinical pharmacology. Academic groups continue dissecting the molecule’s detailed action in various organs, hoping to block pain pathways without stoking heart or digestive system problems. Recent work in computational chemistry looks to optimize its fit inside target enzymes, seeking custom-tailored analogs that dial efficacy and safety even tighter. Every year, global sales and prescription rates drive new clinical studies, pushing for broader access with gentler long-term effects.
Toxicity Research
No medication escapes scrutiny, and Ketoprofen’s profile draws special focus for long-term toxicity and overdose danger. Animal studies confirm high doses will strain the stomach lining, liver, and kidneys—mirroring the risks in human case reports. Researchers note that even moderate courses may boost blood pressure in sensitive people, or interfere with asthma management. Long-standing data tracking thousands of patient-years make clear that complications from GI ulceration or kidney injury stay rare with the right supervision and checkups. Monitoring for skin reactions, especially in sun-exposed patients, picks up another slice of risk in everyday practice. Current guidelines reflect these realities, placing trust in education and doctor-patient communication to keep side effects rare and manageable.
Future Prospects
Demand for effective pain relief powers ongoing Ketoprofen innovation. Scientists explore ways to combine it with safe gastric protectants or deliver it straight to inflamed joints with nanocarriers, aiming to cut down the overall drug load. Industry pushes new transdermal patches and dissolving films that work fast and skip gut irritation altogether. Meanwhile, pressure for greener chemistry in the manufacturing pipeline inspires cleaner synthesis, better waste control, and sustainable sourcing of raw materials. With a strong spot in treatment guidelines and generations of clinical evidence, Ketoprofen will keep evolving alongside new discoveries in pain science and patient care.
What is Ketoprofen used for?
Pain Relief People Rely On
Pain can knock the wind out of your day. People use ketoprofen because it tackles pain right at the source. Over the years, both doctors and folks struggling with arthritis, muscle aches, or sprains turn to it for its ability to take the edge off pain and bring swelling down. This isn’t just about toughing it out—chronic pain steals moments from daily life, slows you down, and wears on mental health. So, bringing down pain helps more than just the body. It gives people back time to focus on the things that matter.
How It Works
Ketoprofen falls in the group of medicines called nonsteroidal anti-inflammatory drugs (NSAIDs). It blocks certain substances in the body—called prostaglandins—that your nerves use to shout, “Something's hurting here!” The science is solid: with lower prostaglandins floating around, both the pain and swelling ease up. For people with arthritis, that’s a big deal. The swelling and stiffness from daily inflammation can make even simple tasks feel tough. A medicine like ketoprofen, in a pill or topical gel form, gives many a better shot at moving about and handling their routines.
Why This Medicine Matters
Too often, folks accept a lower quality of life because painkillers don’t work well or cause problems. There are plenty of horror stories about opioid addiction. Unlike strong opioids, ketoprofen doesn’t create a risk of addiction in the same way. Many doctors lean toward NSAIDs for this reason, especially for conditions like low back pain, osteoarthritis, or menstrual cramps. Multiple studies, including research in the British Journal of Clinical Pharmacology, show that ketoprofen stacks up well against old standards like ibuprofen or naproxen—and sometimes even beats them for certain types of pain.
Access to an option like ketoprofen takes some anxiety out of managing pain. People who can’t tolerate one NSAID sometimes do fine with another, so trying ketoprofen may give relief that acetaminophen can’t.
What Doctors Watch Out For
Every medication has a list of side effects. Not everyone should use ketoprofen, especially folks who deal with stomach ulcers, kidney trouble, or heart concerns. It can lead to stomach irritation, bleeding, or worse if someone ignores the warning signs. So, experienced health professionals look at the big picture—family history, other medications, and lifestyle. They check for risks before handing out a prescription or suggesting an over-the-counter gel.
People without insurance struggle to cover the cost of brand-name versions, but generic forms keep it more accessible. Consumers should read labels, follow dosing instructions, and talk about any new or weird symptoms with a health provider. That stops little problems from turning into big ones.
Better Options for Tough Lives
The need for smart, safe, and affordable pain relief stands out in a world where many folks face chronic illness. Not every medicine works for everyone, but ketoprofen offers choices for those searching for a life with less pain and stiffness. Doctors and pharmacists have a duty to keep up with changing guidelines. Patients can ask questions about risks, long-term plans, and alternatives instead of feeling rushed out the door. Open conversations mean better results and fewer regrets. The power lies in not giving up the search for comfort, one day at a time.
What are the side effects of Ketoprofen?
Ketoprofen: More Than Just Pain Relief
Pain sends people searching for quick fixes, and nonsteroidal anti-inflammatory drugs like ketoprofen land on the list pretty often. I’ve listened to folks at the pharmacy counter griping about sore knees and aching backs, and they count on these pills to help them keep moving. Yet, for all the popularity, the side effects deserve real attention. Not everyone reads the fine print that comes in the box, but in my experience, understanding what can go wrong often helps people make better choices about their health.
Common Body Reactions You Can't Ignore
Stomach trouble tops the chart with ketoprofen. Whether it’s mild heartburn after a single dose, or something harsher like stomach ulcers after days of use, the risk gets real, especially as people age or mix it with other pain relievers. Statistics show that NSAIDs, as a group, cause over 100,000 hospitalizations in the U.S. every year mostly for stomach bleeding. Ketoprofen is no exception. My uncle once ended up in the ER with a bleeding ulcer after taking these meds for his arthritis—he thought the worst side effect he’d get was a little heartburn.
Gut issues only scratch the surface. Ketoprofen can spark kidney trouble, too. Whether it’s dehydration from too little water during hot months or ongoing use in older folks, the kidneys sometimes struggle to process NSAIDs. Sudden weight gain, swollen ankles, or feeling out of breath can signal kidney injury, and these symptoms often go unnoticed until they get serious. People with high blood pressure or diabetes face even bigger risks.
Risk Runs in the Bloodstream
Popping NSAIDs like ketoprofen for too long stacks the odds against your heart. Studies over the past couple of decades connect these medicines to an increased chance of heart attack and stroke, especially for those with pre-existing heart disease. It doesn’t seem fair—a pill meant to help aching joints making things harder for the heart. I remember a neighbor who tried to tough out a marathon training cycle with ketoprofen, only to land in cardiology after chest pains. The lesson stuck: even over-the-counter drugs can have long-range consequences.
Allergic Reactions and Unpredictable Responses
Some people run into hives, swelling, or even difficulty breathing. Allergic reactions, though less common, can be life-threatening. Asthma sufferers seem to have higher odds, and I’ve seen it happen in clinics. Red eyes, itching, and rashes are early warning signs—dismiss them, and you might see something worse.
Looking for Smarter Choices
Doctors point out that using ketoprofen at the lowest possible dose, for the shortest time, cuts the chances of bad side effects. Protecting the stomach with food or medication like proton pump inhibitors helps, but doesn’t give a free pass. Checking in with a pharmacist or doctor about your medical history—things like past ulcers, kidney disease, or heart problems—prevents a lot of suffering. Prescription painkillers aren’t the only option; alternatives like physical therapy, heat, or acupuncture may reduce reliance on pills altogether.
Paying attention to side effects supports better choices—whether for yourself or someone you care for. Health doesn’t come in a bottle, and stories from real life back up the warnings science gives us. Reading every label before popping a pill can save a lot of trouble down the road.
How should I take Ketoprofen?
Understanding Ketoprofen’s Role
Most people looking for relief from arthritis aches or muscle pain stumble across ketoprofen. This medicine fights inflammation and lowers pain. Doctors tap ketoprofen for short-term relief, especially after sprains, surgery, or dental work. My dad once used it for his knee after a hiking accident, and it really brought down the swelling fast.
Using Ketoprofen Safely
Always talk to your doctor before starting ketoprofen. That includes over-the-counter versions. Don’t double up on painkillers—mixing ketoprofen with other NSAIDs like ibuprofen or aspirin boosts the chance of stomach problems.
Ketoprofen comes in capsules, tablets, gels, and creams. Pills usually go with a glass of water. Stomach upset? Food or milk can settle things. Some folks get sleepy or dizzy, so driving right after won’t work.
Dosing isn’t the same for everyone. Age, weight, and any health problems play big roles. For adults, doctors usually say one pill every six to eight hours, but never more than your doctor says. Kids and seniors need smaller doses to dodge stomach bleeding and other trouble.
Missed a dose? Skip it if the next one’s close. Doubling up won’t do you any favors. Spacing out every dose as directed keeps your pain managed without raising your risk.
Watching for Side Effects
No painkiller leaves you totally risk-free. Ketoprofen can upset the stomach, cause headaches, or bring on rashes. My own uncle tried it for back pain and ended up with a rash, so everyone reacts differently.
Big stomach pains, black stools, or trouble breathing count as emergencies. Call your doctor fast if these show up. Drinking alcohol or smoking while taking ketoprofen ramps up bleeding risks, so it pays to be careful.
Long-Term Use Matters
NSAIDs work well for short stretches, not forever. Doctors warn against long-term daily use. Extended runs raise the risk of ulcers, kidney mess-ups, and even heart problems, especially in people with blood pressure issues.
To cut these risks, use the lowest dose that works, for the shortest time possible. Regular follow-ups with your doctor let you track any trouble spots. Blood tests sometimes catch kidney or liver problems early, a smart move if you need this medicine often.
Improving How We Use Painkillers
Pain rarely has a single solution. Heat packs or gentle exercise sometimes work better than extra medicine. I watched my neighbor with arthritis join a gentle yoga class and find much better relief than relying on pills alone.
Pharmacists give solid tips on how to juggle different medicines. Instead of toughing it out alone, use these resources. Always store ketoprofen away from kids and check expiration dates every few months.
Clear conversations with doctors cut down mistakes and keep side effects at bay. Paying attention and speaking up goes a long way. When pain hits, smart choices about medicine like ketoprofen help us bounce back, work, and rest easier.
Can I take Ketoprofen with other medications?
Looking Beyond the Pill Bottle
Back pain, headaches, arthritis—these aches push many people toward over-the-counter relief like Ketoprofen. This nonsteroidal anti-inflammatory drug (NSAID) has been in medicine cabinets for years. Folks reach for it because it cuts pain and combats swelling. But health rarely travels a straight path. Most people dealing with chronic discomfort also take other medicines. That’s where things can get tricky.
Real Risks of Drug Combinations
Every pharmacy counter holds stories. I recall working in a busy city pharmacy and seeing customers who relied on several prescriptions each day. People often believe that if two drugs come from a doctor or the local store, they work safely together. The reality: Ketoprofen can clash with other medications in unpredictable ways.
Blood thinners bring the biggest concern. Aspirin, warfarin, or clopidogrel manage blood clots or heart conditions, but combining any of them with Ketoprofen raises the risk of serious bleeding. Stomach ulcers develop more easily and internal bleeding sometimes happens with no warning. I once had a patient call in with dark stools, thinking it wasn’t serious. It turned out his stomach was bleeding after mixing his daily aspirin and Ketoprofen for just one week.
High blood pressure and heart failure medications deserve attention, too. Diuretics and ACE inhibitors keep these conditions stable, but Ketoprofen sometimes blocks the effect, leading to fluid retention or raised blood pressure. Patients who depend on lithium for mood disorders also walk a tightrope since NSAIDs may push lithium levels so high that confusion and even seizures creep in.
The Unique Ways Bodies React
No two people respond to medicine in quite the same way. Age plays a role—older adults process drugs more slowly. The kidneys handle a big part of the workload, and they can struggle with too many tasks. If kidneys start to falter, Ketoprofen may stick around the body longer than intended. This increases the risk for toxic build-up, and silent kidney damage can progress for months without obvious symptoms.
Reading Labels Isn’t Enough
Instructions and warning labels appear simple, but mixing medications takes more than a glance at a leaflet. Doctors and pharmacists train for years on drug interactions, but they rely on accurate lists from patients. Sharing every supplement or herbal remedy counts, too. Fish oil, for example, seems harmless, but at high doses it can thin the blood and add to Ketoprofen’s risks.
What Helps People Stay Protected
People can avoid trouble with the right routines. Keep a written list of everything you take and bring it to all appointments. If you ever need to start Ketoprofen, check with a health care provider or pharmacist about the safety of each combination. Online drug interaction checkers offer useful information but never capture the whole picture—the subtleties of illness, age, and kidney function need a personal touch.
Beyond that, watch for warning signs: blood in the stool, strong stomach pain, shortness of breath, swelling in the legs, confusion, or sudden headaches. These signals warrant attention right away. Simple, open conversations with a care team can head off disaster before it starts. Years watching people’s lives improve—or unravel—have taught me that managing drug combinations is about honesty, vigilance, and real teamwork.
Is Ketoprofen safe during pregnancy or breastfeeding?
What Doctors Say About Ketoprofen Use
Pregnancy and breastfeeding both bring a lot of joy, along with a tidal wave of questions about what is safe for a parent and their baby. Pain relief becomes a tricky topic. Ketoprofen, a non-steroidal anti-inflammatory drug (NSAID), often gets mentioned alongside familiar names like ibuprofen and naproxen. It reduces swelling and knocks down fevers, yet the conversation changes the moment pregnancy or breastfeeding enters the picture.
Digging Into the Science
Obstetricians warn against most NSAIDs after 20 weeks of pregnancy, including ketoprofen. Research points to a risk of low amniotic fluid and kidney issues in developing babies. Studies published in medical journals have shown that using these drugs, especially closer to the third trimester, can also affect a baby’s heart. The fetal ductus arteriosus, a blood vessel critical for fetal circulation, might close too soon, leading to serious complications.
Some data covers earlier stages of pregnancy as well. Reports from the American College of Obstetricians and Gynecologists suggest avoiding NSAIDs like ketoprofen in the first trimester since they may increase the chance of miscarriage. The evidence is not always clear-cut, yet the stakes are high.
Real-World Experience Matters
Expectant parents, myself included, know how tempting pain pills can get. Backache, headaches, the all-night tossing—pregnancy brings aches that Tylenol sometimes barely touches. I remember reaching for over-the-counter medicines and putting the bottle back on the shelf, unsettled by the warning label. Chatting with pharmacists and doctors, I learned that acetaminophen usually offers a better choice when painkillers can’t be skipped. It’s not risk-free, but doctors have studied it more and tend to feel comfortable recommending it in pregnancy, whereas ketoprofen stays on the restricted list.
Breastfeeding and Medicine Transfer
The concerns shift for breastfeeding. Medication leaks into breast milk, passing small amounts on to babies. While ketoprofen makes it through in only tiny traces, the long-term effects have gaps in research. Health authorities in Europe and North America both recommend caution. While a single dose probably won’t trigger an emergency, regular use leads to more uncertainty. Newborns break down medicines more slowly, which means a day-old infant faces higher risks from lingering medicine in milk than an older baby.
Why Knowing Matters
Half of all pregnancies are unplanned, so people sometimes rely on painkillers before they know a baby is on the way. Every new parent deserves clear, honest information from experienced healthcare workers, not just a list of warnings. The best defense comes from routine conversations with pharmacists and doctors. If a parent needs more than an occasional mild pain reliever, clinicians often steer them toward alternatives—like restorative sleep, gentle exercise, and non-medicine remedies for swelling.
Alternatives and Preventing Risk
Health professionals recommend reaching for acetaminophen if relief is needed, and only in short bursts. For more persistent pain or inflammation, physical therapy and cold packs help a surprising number of people. For chronic conditions, even before conception, regular reviews with a rheumatologist or pain specialist can map out a plan that supports both parent and baby.
Education helps. Prenatal classes now cover medicine use. Pharmacies point out safer choices, and care teams encourage open questions. No parent should feel shamed for seeking relief, but understanding the unique risks of specific drugs, like ketoprofen, often keeps babies safer from the start.
| Names | |
| Preferred IUPAC name | (RS)-2-(3-benzoylphenyl)propanoic acid |
| Other names |
Ketonal Oruvail Fastum Actron Ketoprofenum Profénid OKI Orudis Flexen |
| Pronunciation | /kiːˈtoʊ.prə.fɛn/ |
| Identifiers | |
| CAS Number | 22071-15-4 |
| Beilstein Reference | 83262 |
| ChEBI | CHEBI:6120 |
| ChEMBL | CHEMBL476 |
| ChemSpider | 5463 |
| DrugBank | DB01009 |
| ECHA InfoCard | 100.043.285 |
| EC Number | 2.3.1.180 |
| Gmelin Reference | 1593748 |
| KEGG | D08006 |
| MeSH | D007668 |
| PubChem CID | 3826 |
| RTECS number | UJ5510704 |
| UNII | 6COU62GI7I |
| UN number | UN2811 |
| Properties | |
| Chemical formula | C16H14O3 |
| Molar mass | 254.28 g/mol |
| Appearance | White or almost white crystalline powder |
| Odor | Odorless |
| Density | 1.13 g/cm3 |
| Solubility in water | Slightly soluble |
| log P | 3.12 |
| Vapor pressure | 5.85E-7 mmHg |
| Acidity (pKa) | 4.45 |
| Basicity (pKb) | 5.94 |
| Magnetic susceptibility (χ) | -77.5×10⁻⁶ cm³/mol |
| Refractive index (nD) | 1.576 |
| Dipole moment | 2.20 D |
| Thermochemistry | |
| Std molar entropy (S⦵298) | 274.0 J·mol⁻¹·K⁻¹ |
| Std enthalpy of formation (ΔfH⦵298) | -390.8 kJ/mol |
| Std enthalpy of combustion (ΔcH⦵298) | -6447 kJ/mol |
| Pharmacology | |
| ATC code | M02AA10 |
| Hazards | |
| Main hazards | Causes serious eye irritation. Causes skin irritation. May cause an allergic skin reaction. |
| GHS labelling | GHS07; GHS08; Warning; H302, H315, H319, H351, H373 |
| Pictograms | pregnancy-warning|acetaminophen-allergy|kidney-warning|liver-warning|stomach-warning|drowsiness-warning|driving-warning|alcohol-warning|prescription-only |
| Signal word | Warning |
| Hazard statements | H315: Causes skin irritation. H319: Causes serious eye irritation. H335: May cause respiratory irritation. |
| Precautionary statements | Keep out of reach of children. Avoid contact with eyes, mucous membranes and broken skin. Wash hands thoroughly after handling. If swallowed, get medical help or contact a Poison Control Center right away. Use only as directed. |
| NFPA 704 (fire diamond) | Health: 2, Flammability: 1, Instability: 0, Special: |
| Flash point | 42°C |
| Autoignition temperature | 472°C |
| Explosive limits | Lower: 0.7% Upper: 5.0% |
| Lethal dose or concentration | LD50 oral rat: 360 mg/kg |
| LD50 (median dose) | LD50 (median dose) of Ketoprofen: 360 mg/kg (oral, rat) |
| NIOSH | RG6300000 |
| PEL (Permissible) | PEL: Not Established |
| REL (Recommended) | 100 mg |
| IDLH (Immediate danger) | No IDLH established. |
| Related compounds | |
| Related compounds |
Ibuprofen Naproxen Fenoprofen Flurbiprofen Dexibuprofen Carprofen Fenbufen |