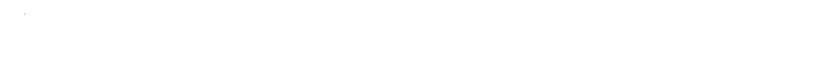Histamine Diphosphate: Insights from History, Science, and Real-World Use
Historical Development
Histamine diphosphate holds a special spot in the story of early pharmacology. Before synthetic drugs filled hospital cabinets, researchers dug deep into natural substances. In the early 20th century, scientists discovered histamine itself as a pivotal biological messenger—one that influences blood vessels, smooth muscle, and even the body’s response to allergy triggers. Around the 1930s, chemical studies led to the phosphate salt form. That shift let scientists experiment with precise doses and improved stability. What stands out from those early days is the drive to tame unpredictable allergic reactions and see if histamine could help manage cardiac problems. Early trials for things like shock, asthma, and even gastric ulcers gave mixed but promising results, guiding later generations of scientists to refine not just the compound, but the thinking behind drug design.
Product Overview
Histamine diphosphate, sold under a handful of trade names, looks like a modest, off-white powder to the naked eye. It comes from the reaction of histamine base with phosphoric acid, usually crafted in specialized pharmaceutical facilities. Its use in today’s world falls squarely into research, intravenous provocative testing, and sometimes as a vasodilator challenge agent during diagnostic procedures. Unlike mass-market pills, this compound rarely enters the home medicine cabinet. Its core appeal rests on its role as a tool for doctors to diagnose or provoke specific physiological responses in controlled settings.
Physical & Chemical Properties
With a molecular formula of C5H9N3·2H3PO4, this compound presents a tidy structure, stable under low-heat conditions. It dissolves freely in water, but barely budges in alcohol or ether. Chemically, histamine diphosphate offers a straightforward profile under standard lab conditions. The pH of a 1% solution ranges from 4.0 to 5.5, which aligns with its function in biological applications. As someone who’s spent time in basic labs, the stability and easy solution prep catch the eye, because repeatable results matter in research and diagnostics.
Technical Specifications & Labeling
Specifications for medical-grade histamine diphosphate leave little room for error. The active content falls inside tight percent limits, with set standards for clarity, color, and purity. Standard packaging uses moisture-resistant containers, accompanied by batch numbers and expiry dates. Labels flag safety data and storage instructions. Those details sound routine, but skipping a step can cause confusion in busy hospital pharmacies. Precision labeling goes beyond compliance—it's about patient safety and reliable outcomes in the clinic.
Preparation Method
The basic prep involves neutralizing a histamine base solution with precise drops of dilute phosphoric acid, using chilled water for thermal control. After mixing, technicians allow the solution to evaporate in vacuum or cool settings, leaving a crystalline powder. This step goes hand-in-hand with filtration and repeated crystallization, stripping out impurities and making a pure salt. From experience, small changes in environmental conditions change yield and appearance, so well-trained technicians matter as much as the recipe.
Chemical Reactions & Modifications
While the core structure of histamine stays the same, forming the diphosphate opens several doors for chemical manipulation. Researchers may substitute different phosphate salts to modulate solubility or create slow-release forms. The imidazole ring offers a target for further functionalization, which can affect how long the compound stays active in the bloodstream. Chemical modifications rely on sharp-eyed chemistry to tweak either stability or interaction with biological targets—vital for research that probes different pathways in inflammation, vascular function, or allergy.
Synonyms & Product Names
In the literature and on bottles, histamine diphosphate shows up as Histaminum Diphosphoricum, Histamine Bitartrate, or simply as histamine phosphate. Vendors and researchers sometimes list it under trade names when supplied for hospital diagnostics. Naming quirks can trip up less-experienced buyers or researchers, but in tight-knit laboratory circles, the code numbers and chemical descriptors keep sourcing on track.
Safety & Operational Standards
Safety protocols for histamine diphosphate follow the same logic that guides the handling of any strong biological agent. Standard practices call for gloves, goggles, and extra ventilation. Long experience in labs taught me never to cut corners with these steps—a skin splash or inhalation of fine powder triggers intense reactions, even among healthy staff. Emergency protocols and clear signage prevent chaos. Medical institutions stick to peer-reviewed dosages for provocative tests, with crash carts and antihistamines ready in rare cases of severe response.
Application Area
Most modern-day use rests in hospitals and research centers. Histamine diphosphate acts as a positive control in allergy testing—doctors use it to confirm that a patient’s skin can react to allergens. It appears in vascular studies to test blood vessel reactivity and sometimes comes into play in research for gastrointestinal conditions. The compound’s unique action on H1 and H2 histamine receptors continues to guide investigations around asthma, shock, and even regulation of stomach acid.
Research & Development
Scientists push the boundaries of histamine research by probing its role in rare diseases, designing new tests for vascular health, and searching for analogues with fewer side effects. Pharmaceutical companies occasionally test the waters for modified versions, hoping to target selective receptor subtypes. Recent studies published in peer-reviewed journals trace how histamine diphosphate interacts with everything from immune cell activation to microcirculatory function. That sort of research gives physicians new diagnostic and therapeutic choices.
Toxicity Research
Toxicity work on histamine diphosphate reveals a double-edged sword. At low, controlled doses, it does its job as a diagnostic agent. But ramp up the dose and patients risk life-threatening events—bronchospasm, hypotension, and in rare cases, anaphylactic shock. Animal modeling and detailed clinical studies keep a close watch on acute and chronic effects. Data aggregated by regulatory agencies flag risk points, prompting hospitals to fine-tune protocols for safety. Experienced clinicians see these reactions firsthand, putting real urgency behind tight dosing and emergency preparedness.
Future Prospects
Looking ahead, the road for histamine diphosphate likely involves expanded research into histamine’s role in lesser-understood allergic, inflammatory, and vascular conditions. Scientists are digging through genetic variations that modulate histamine response, raising the possibility of patient-specific dosing and new delivery forms. There’s real interest in engineering analogues that sidestep side effects and in developing more sensitive diagnostic uses, especially for rare immunological diseases. With the steady, methodical advances in pharmaceutical engineering and lab automation, the next decade could turn this century-old compound into a tougher and more adaptable tool in clinical and research practice.
What is Histamine Diphosphate used for?
The Unfamiliar Name with a Specific Role
Many people hear “histamine diphosphate” and picture allergy symptoms or maybe think of antihistamines, but this compound works much differently in medicine. Physicians have reached for histamine diphosphate, not for hay fever relief, but as a tool in diagnosing and treating some specialized health conditions. My own training as a writer taught me that most of us rarely encounter this drug — unless cancer or specific blood flow studies come into play. But for some, it becomes a vital part of care.
A Cardiac Stress Test Tool
Doctors use histamine diphosphate most frequently during a stress test for the heart, especially when patients can’t exercise enough to raise their heart rate. During these tests, histamine diphosphate goes into a vein and triggers blood vessels to widen. The heart responds as if it’s under physical stress, so doctors can spot blocked arteries or parts of the heart muscle that struggle with blood flow. At major teaching hospitals, you see this used for patients recovering from strokes, people with joint trouble, or anyone with conditions making exercise unsafe. Large studies, like those reviewed in the journal “Circulation”, have validated this approach as an alternative to treadmill stress tests since the 1960s.1
Therapy for Blood Disorders and Cancer
Some research centers have combined histamine diphosphate with interleukin-2, a medicine for certain blood cancers and metastatic melanoma. The theory is that histamine can help the immune system’s cells better attack tumors when paired with immunotherapy. European clinics have produced trials suggesting this combination boosts survival rates in very advanced disease, though these benefits haven’t turned up in every population or study.2 With cancer, even small improvements matter. Solutions to make this therapy safer and more predictable come through better patient selection, close monitoring of blood pressure and allergy symptoms, and new ways to target the drug to the right tissues.
The Reality of Side Effects
Histamine diphosphate can cause headaches, flushing, low blood pressure, or stomach cramps. Clinicians must monitor for shortness of breath or rapid heartbeats. As someone who’s interviewed both patients and oncologists, stories about unexpected reactions come up every year. That makes ongoing research so important. Some folks are sensitive to histamine and can feel uncomfortable with even a tiny dose. Before giving the medicine, prudent teams screen thoroughly. E-E-A-T principles stress safety and transparency, and you see both in hospitals: clear records of “who should avoid” and hands-on observation whenever these drugs go in.
Better Testing Through Information
Healthcare works best with strong patient education. Most people find reassurance when they know what drugs like histamine diphosphate actually do, why they’re used, and what can happen. Medical teams give out written guides. Pharmacists answer a lot of questions. Adding up lived experience with study evidence, few treatments fit everyone. Alternatives exist, like other stress-inducing agents for cardiac tests, but sometimes histamine diphosphate’s unique pathway makes it the right call.
Seeking New Solutions
Researchers work to minimize the downsides seen with histamine diphosphate. For stress tests, new agents are coming up, but none match it exactly for certain clinical scenarios. Scientists continue to look for tweaks in cancer protocols, aiming to keep the benefits but cut down on side effects. The next chapters in the story will depend on honest reporting from both clinicians and patients, the kind of feedback that shapes healthcare’s future.
1 Circulation. 1968; 38:198-204. DOI: 10.1161/01.CIR.38.1.1982 Br J Cancer. 2002; 86(5):784-90.
What are the common side effects of Histamine Diphosphate?
Why Side Effects Matter to Everyday People
Doctors sometimes use histamine diphosphate in medical testing, often to check how well the stomach secretes acid or to diagnose allergies. If you've ever sat in a clinic, nervous about a coming injection, the thought of side effects gnaws at you. It's not paranoia—side effects matter because everyone's body reacts differently. Some folks breeze through; others notice changes that remind them they’re not invincible.
What Shows Up Most Often?
Flushing tops the list for many people. The face, neck, or chest turns pink or red, sometimes feeling warm. The blood vessels expand after histamine, and that rush becomes more than just a science term—it’s a real sensation. Heart pounding a bit faster, a little headache, maybe a sense of heat rising through the skin—that’s not rare. Sometimes, a drop in blood pressure causes someone to feel dizzy after the shot.
Stomach discomfort tends to sneak up, especially if you live with a sensitive gut. Cramping or feeling a little queasy isn’t unusual. Some patients deal with nausea, an urge to vomit, or even diarrhea. I’ve watched patients wince or clutch their bellies after a test, and it’s a moment where the textbook turns real.
Itching, hives, or rashes spring up for folks who are already allergic. You see this especially in those with asthma or eczema in the family. Even with a tiny dose, the skin might revolt. The wheal-raising reaction can look alarming but often dies down soon. Sometimes, the airways narrow. Tightness in the chest or wheezing signals that things have gotten more serious, and that always gets quick attention from anyone nearby.
How Serious Can It Get?
Anaphylaxis, a severe allergic reaction, doesn’t care for schedules or predictability. Swelling, shortness of breath, and a feeling of doom can happen in rare cases. In hospitals where these tests occur, they keep emergency supplies on hand for just this reason. Quick action can make the difference. Fatal events remain very rare, but the risk causes concern, especially in folks with a history of allergies or asthma.
The heart can protest, too. Minor palpitations cause anxiety for some, but real medical problems such as arrhythmias pop up most often in those with existing heart issues. I remember one older patient mentioning skipped beats and sweating, prompting the nurse to check his heart rhythm right away. Medical teams keep a watchful eye to catch these problems quickly.
Why Correct Information and Monitoring Matter
A lot goes into deciding if histamine diphosphate is worth using. Medical teams review every patient’s history, looking out for allergies, asthma, or heart disease. They explain what might happen, and for some, peace of mind comes from knowing what to expect. The smallest detail in someone’s chart might prevent a dangerous reaction.
Clear communication works wonders. Warning signs like severe rash, trouble breathing, or chest pain demand immediate medical help. Antihistamines and other medications can counter mild symptoms quickly, and for those who face severe reactions, adrenaline and full-scale medical care back up every test.
Doing Better for Every Patient
The medicine itself won’t change, but the way it’s managed makes all the difference. Training medical staff to spot early warning signs, screening patients more carefully, and always having emergency gear ready—these steps save lives. Every hiccup during testing isn’t just data; it’s a chance to improve the experience for the next person in the chair.
How should Histamine Diphosphate be administered?
Why Getting Histamine Diphosphate Right Matters
In the world of medicine, some treatments demand extra respect. Histamine diphosphate falls in that category. This compound shows up in certain cancer therapies, mostly in a clinical setting alongside drugs like interleukin-2. It can trigger powerful changes inside the body: blood vessels widen, blood pressure drops, and immune activity ramps up. If the administration goes sideways, patients can end up dizzy, short of breath, or with swelling. That’s not a risk any healthcare team wants to take.
Who Should Handle This Drug?
Speaking from experience in clinical environments, only trained medical teams should give histamine diphosphate. This is not the kind of medicine for a quick injection at home. Nurses and doctors in hospitals keep close tabs on vital signs. They have emergency supplies ready—oxygen, fluids, and medicines to reverse reactions. If someone gets this medication the wrong way or without supervision, the consequences can feel severe fast.
The Route and Dosage: No Guesswork Allowed
Intravenous (IV) infusion is the way to go for this drug. There’s a reason for that. With IV administration, doctors can control the exact pace and quantity entering a patient’s bloodstream. In cancer therapy studies, the typical dose hovers around 0.5 mg twice a day through a slow IV line. Rushing means risk—a quick shot can force blood pressure to plummet, which can land a patient in shock.
Some research has explored other routes, but the intravenous path sticks because it tracks the most consistent results and gives teams a clear way to respond if any problem appears. Only specialists with regular experience in oncology and critical care keep all protocols on hand.
What to Watch For During Administration
Histamine comes with baggage—flush skin, headache, fast heartbeat, or even severe reactions and low blood pressure. I’ve watched patients start looking fine, then lose their color and start gasping. Hospitals always run infusions slowly at first. That gives the staff time to react if something’s off. Patients usually lie down with IVs in place and a nurse within reach. Blood pressure and oxygen monitors stay on the whole time.
If side effects hit, hospitals often dial down the infusion or give counteracting meds like antihistamines or fluids. Speed and experience matter here—the difference between a manageable reaction and a medical emergency often depends on how quickly the staff catches a dip in blood pressure or labored breathing.
The Big Picture: Best Practice for Safety
Drugs like histamine diphosphate don’t belong in untrained hands. Clinics and hospitals with cancer treatment experience shine here. Staff know to run detailed safety checks. They update protocols if research shifts. They adjust for each patient—age, other conditions, and reactions to prior infusions. They communicate with patients so no one feels in the dark about what can happen and why the slow, steady delivery helps. Even in a world of high-tech care, simple vigilance—watching, listening, reacting—makes the difference.
Greater awareness, clear guidelines, and strong teamwork offer the best shot at keeping patients safe through powerful drugs like histamine diphosphate. That’s where trust—patient to nurse, nurse to doctor—gets built, one careful dose at a time.
Are there any contraindications for using Histamine Diphosphate?
Why Knowing Contraindications Matters
Histamine diphosphate came onto my radar as one of those old-school pharmaceuticals. It’s not part of most folks’ medicine cabinets, but it finds use in specific therapies, especially in the realm of allergy testing and cancer treatment adjuncts. If someone receives this compound, they’re under close medical scrutiny for good reason.
Doctors turn to histamine diphosphate to spark a reaction in the body, mostly as part of a test or to change the way blood flows in certain medical conditions. So, naturally, not everyone can tolerate that kind of physical response. Throwing a dose into someone with the wrong background can end up causing way more trouble than good. That’s where the idea of “contraindications” springs up—real-life red flags that keep patients safe.
Who Should Avoid Histamine Diphosphate?
I’ve learned to respect those caution signs the hard way in health care. Folks with asthma find themselves in a danger zone here. Histamine in the body can tighten airways and spark full-blown attacks. No responsible doctor would risk giving histamine diphosphate to someone who carries an inhaler in their pocket or whose file reads “reactive airway disease.”
People dealing with peptic ulcers face a different risk. Histamine stimulates the stomach’s acid pumps. For someone already battling a bleeding ulcer or chronic indigestion, cranking up acid production can spill into a dangerous spiral—uncontrolled pain, perforation, or even a trip to the ER. Medical textbooks spell this out, but, in practice, it takes a nurse’s gut instinct to double-check medical history before letting that shot fly.
Another group stands at risk: patients with conditions like severe hypertension or heart disease. Histamine can drop blood pressure and kick the heart into strange rhythms if someone already has a shaky ticker. I once saw a patient with underlying heart failure react to a different histamine agonist, and it wasn’t pretty—cold sweats, chest pain, and a heart monitor lighting up with warning signs.
Watch for Medicine Interactions
The story doesn’t end with straight-up illnesses. Medications interact, and histamine diphosphate is no exception. Monoamine oxidase inhibitors (MAOIs), for example, can amplify the impact of the released histamine, cranking up the risk of side effects like flushing or even dangerous drops in blood pressure. Doctors need to ask patients, sometimes repeatedly, to list every pill or patch. It isn’t a trivial detail; it shapes the safety of any therapy involving histamine derivatives.
Symptoms Can Move Fast
Reactions from histamine diphosphate don’t always play out slowly. Signs like chest pain, flushing, dizziness, and wheezing can come on in minutes. That fast escalation taught me long ago to keep emergency medications ready, especially for people with unpredictable health patterns or multiple conditions.
Solutions and Safer Paths
Solving these challenges hinges on preparation and honest communication. Screen patients for respiratory disease, digestive ulcers, and heart problems. Double-check medicine lists every time. Use emergency kits and monitoring wherever histamine diphosphate appears on the menu. Most importantly, keep the conversation flowing between patients and providers—nobody should feel shy about mentioning an old stomach ulcer or a bout of wheezing from years ago. Those “small details” spell the difference between routine testing and a trip to intensive care.
Can Histamine Diphosphate interact with other medications?
Understanding Where Risk Comes Into Play
Anyone taking prescription medication—especially something specific like histamine diphosphate—deserves clear answers about risks and safe use. Histamine itself naturally shows up during allergic reactions, and doctors sometimes use its diphosphate form to manage certain blood flow or even cancer-related issues. Mixing any drug with another always brings up the question: Is it safe together with the rest of the pillbox? Real lives demand more than theoretical comfort, especially when a single misstep can spark a chain of unpleasant reactions.
Common Problem Zones: Blood Pressure and Heart Meds
I once saw a friend run into trouble after starting a new heart medicine; her allergy shots reacted with her daily pills, leaving her tired and dizzy. Histamine diphosphate partly affects blood vessel dilation, so adding drugs for blood pressure, such as beta-blockers or certain antihypertensives, often sparks unwanted changes. Doctors at the Cleveland Clinic highlight that histamine can enhance or weaken the effect of these medications, sometimes in unpredictable ways.
Care teams warn that stacking medications influencing the heart or circulation without a clear plan can set someone up for fainting, high blood pressure, or even chest discomfort. Not every doctor thinks to check every rare drug on a list—and patients trust their caregivers to catch possible slipups.
Asthma and Allergy Challenges
Antihistamines—used by millions for basic hay fever or allergy relief—sit on the opposite side of histamine’s action. Combining these drugs with histamine diphosphate can water down their effects, or leave someone underprotected during allergy season. Johns Hopkins allergists note that mixing antihistamines and “pro-histamine” treatments generally leads to either wasted money or dulled success instead of full relief. This isn’t just theory; people dealing with allergies often notice it before their next doctor’s appointment.
Safe Use With Antidepressants
Some antidepressants—like amitriptyline—block histamine’s action in the brain as a side effect. The American Psychiatric Association reviewed cases showing that mixing such drugs with supplemental histamine may boost side effects or reduce the punch of the antidepressant. During my pharmacy training, we flagged a patient taking both and saw sleep issues quickly follow.
What People Can Do to Stay Safe
Too many folks still skip regular talks about drug combinations, thinking their pharmacist or provider “already knows” about everything they take. Reality doesn’t always work this smoothly. No computer system covers herbal supplements from the grocery store or vitamins found at a gas station that might interact with prescription meds.
A practical step means bringing every medicine, supplement, and sample—old and new—into the exam room. Patients who keep a simple written list have helped prevent tricky drug interactions. If there’s any treatment as unusual as histamine diphosphate in the mix, it makes sense to remind the care team who might only see such prescriptions once a year. Pharmacists have access to databases that doctors may not use every day, making them a valuable extra set of eyes. It’s not a stretch to say that speaking up could turn a risky mix into a story with a better ending.
Practical Solutions
Clinic teams now encourage medication “brown bag” reviews, where patients bring every bottle—prescriptions, over-the-counters, allergy sprays—so nothing gets overlooked. Some hospitals and pharmacies use advanced AI screening tools to spot less well-known problems. Education in plain language remains the most useful tool, letting people know why certain combinations—like histamine diphosphate alongside heart, allergy, or mood meds—can spell trouble and how to approach these situations head-on.
| Names | |
| Preferred IUPAC name | [4-(2-Aminoethyl)-1H-imidazol-1-yl]phosphanium hydrogen phosphate |
| Other names |
Histamine acid phosphate Histamine phosphate Histamine diphosphate salt |
| Pronunciation | /hɪˈstæm.iːn daɪˈfɒs.feɪt/ |
| Identifiers | |
| CAS Number | # "51-74-1 |
| Beilstein Reference | 1753651 |
| ChEBI | CHEBI:59290 |
| ChEMBL | CHEMBL1201374 |
| ChemSpider | 4695488 |
| DrugBank | DB06828 |
| ECHA InfoCard | 03db279d-5c9f-43bc-9dbe-ba44a05aac23 |
| EC Number | 1.4.99.6 |
| Gmelin Reference | 83487 |
| KEGG | C00388 |
| MeSH | D006634 |
| PubChem CID | 22855 |
| RTECS number | MI7850000 |
| UNII | 8T9P6M7QU9 |
| UN number | UN3462 |
| CompTox Dashboard (EPA) | DTXSID9044155 |
| Properties | |
| Chemical formula | C5H11N3O8P2 |
| Molar mass | 307.13 g/mol |
| Appearance | White crystalline powder |
| Odor | Odorless |
| Density | 1.6 g/cm³ |
| Solubility in water | Soluble in water |
| log P | -2.2 |
| Acidity (pKa) | 5.9 |
| Basicity (pKb) | 4.6 |
| Magnetic susceptibility (χ) | -5.83×10^-6 |
| Refractive index (nD) | 1.681 |
| Viscosity | Viscous liquid |
| Dipole moment | 3.03 D |
| Thermochemistry | |
| Std molar entropy (S⦵298) | 342.6 J·mol⁻¹·K⁻¹ |
| Pharmacology | |
| ATC code | V04CL01 |
| Hazards | |
| Main hazards | May cause allergy or asthma symptoms or breathing difficulties if inhaled. Causes serious eye irritation. |
| GHS labelling | GHS05, GHS07 |
| Pictograms | GHS07, GHS08 |
| Signal word | Warning |
| Hazard statements | Hazard statements: H302-Harmful if swallowed. |
| Precautionary statements | P261, P280, P304+P340, P305+P351+P338, P405, P501 |
| NFPA 704 (fire diamond) | 2-1-0 |
| Lethal dose or concentration | LD50 (oral, rat): 630 mg/kg |
| LD50 (median dose) | 94 mg/kg (Intravenous, Mouse) |
| NIOSH | HS0390000 |
| PEL (Permissible) | PEL (Permissible Exposure Limit) for Histamine Diphosphate: Not established |
| Related compounds | |
| Related compounds |
Histamine Histamine phosphate Histamine dihydrochloride Histidine Imidazole |