5-Fluorouracil: Unraveling a Classic Chemotherapy Compound
Historical Development
Long before the 21st-century push for targeted therapies, scientists set their sights on how cancers turn nutrition into growth. In the 1950s, chemists designed 5-fluorouracil (5-FU) as an experiment in disrupting cancer’s building blocks. The thinking: swap a single atom in uracil – a standard component of DNA and RNA – and cancer cells might stumble. Charles Heidelberger led the earliest efforts, feeding mice this lab-made compound and watching tumors shrink. Doctors soon noticed that 5-FU showed real promise in patients with colon, breast, and various gastrointestinal cancers. Approvals followed in the 1960s, anchoring 5-FU as a backbone of oncologic care since then. The persistence of 5-FU on treatment lists worldwide shows how early chemical tinkering can ripple out for generations in health care, even as cancer science advances.
Product Overview
No one can ignore how broadly 5-fluorouracil finds use across medicine. It comes as white powder or granules, and pharmaceutical companies ship it in tablets, creams, and — most important for many cancer patients — injectable solutions. Dosing typically runs from 250 mg to over 1000 mg per square meter of body surface, depending on the regimen. As injection, 5-FU blends with saline or dextrose to run over a few minutes or several days via infusion pumps. Tube-based delivery lands it inside the bloodstream, letting it circulate to tissues needing the most intervention. For skin-based squamous cell carcinoma or precancerous lesions, creams allow local applications, directly killing abnormal cells without as much effect elsewhere.
Physical & Chemical Properties
Physical testing shows a compound that handles itself well in the lab and at the bedside. With the formula C4H3FN2O2 and molecular weight hovering around 130 g/mol, 5-FU appears as a crystalline white powder that dissolves in water and slightly so in alcohol, offering flexibility during formulation. Its melting point hits about 282-286°C, a signal of its relative stability in pharmaceutical storage. Chemically, it acts as a pyrimidine analog, bearing a close resemblance to uracil, save for a single fluorine atom at position 5 of the ring. That small swap makes a big difference in how the body and tumor cells treat the molecule.
Technical Specifications & Labeling
Manufacturers need to hit certain benchmarks to get 5-FU to market. The compound must test at greater than 98% purity by HPLC, with minimal residues of heavy metals or organic solvents. Labels call for warnings about handling and storage, instructing providers to keep drugs in cool, dry environments and clearly marking cytotoxic status. Boxed warnings underline the risks of bone marrow suppression and the necessity of protective equipment and environmental precautions, considering the impact 5-FU exposure can have on pharmacists, nurses, and cleaning crews. Drug vials also list concentration, preservative content, batch numbers, and expiration dates, so patients and clinicians stay fully informed about what goes into a given dose.
Preparation Method
5-fluorouracil enters the industrial pipeline through a nifty series of chemical steps starting from barbituric acid or uracil itself. The core challenge is introducing fluorine at precisely the fifth position. Most routes rely on direct fluorination of uracil using specialized fluorinating agents, such as Selectfluor or elemental fluorine, under controlled conditions. Reaction by-products and excess reagents get washed away through repeated extractions and crystallizations. For the highest yields, some labs use ruthenium or silver catalysts, dialing in temperature, solvent, and reaction time so impurities stay minimal. The end goal: a crystalline product, dry and pure enough to satisfy regulators who know every milligram counts in the clinic.
Chemical Reactions & Modifications
5-FU itself marks just the start of a maze of chemical possibilities. In the body, it takes on new life through a cascade of metabolic steps: enzymes convert it to various phosphorylated forms, like 5-fluoro-2’-deoxyuridine monophosphate (FdUMP), the real active ingredient that jams DNA synthesis in cancer cells. Chemists also tweak the 5-FU core to produce prodrugs — think capecitabine or tegafur — which hit the bloodstream in milder form and convert into 5-FU right inside tumor cells. This trick often lessens toxicity and boosts how long the drug sticks around, which matters to patients struggling with side effects. On the synthesis side, researchers continue searching for cleaner, safer, cheaper routes to make not only 5-FU but targeted versions laced with other functional groups, improving selectivity and reducing harmful fallout on healthy tissues.
Synonyms & Product Names
Pharmacists and consumers run across 5-fluorouracil under an array of names. The most common is simply “5-FU.” Generic tablets and injectables fill hospital drawers, while branded versions such as Adrucil, Carac (for topical), Efudex, and Fluoroplex appear in prescriptions and research publications. Historical records show earlier identifiers such as NSC-19893, a nod to early US cancer institute registries. Product numbers change from one country’s drug registry to the next, so hospitals often rely on the “5-FU” shorthand to cut through bureaucracy. The root word “fluorouracil” survives as a clue to the molecule’s origins, so no one mistakes its function for more benign cousins in the pyrimidine family.
Safety & Operational Standards
Every hospital, compounding pharmacy, and research lab in the world that handles 5-FU lives by strict safety rules. Occupational exposure by inhalation or skin contact produces real risk: case studies document on-the-job toxicity, from rashes to dangerous drops in blood cell counts, especially if workers lack proper gloves, eye shields, or ventilation. International safety agencies (OSHA, NIOSH, EU’s REACH) mark 5-FU as hazardous, demanding closed-system pumps for infusions, cytotoxic waste bins, protective gear, and regular safety audits. Nurses learn to double-check dosing and alert physicians to early symptoms of overdose, as the window between therapeutic and toxic grows narrow in frail patients. The operational culture puts patient safety first, closely tracking each vial so no errors occur, and running extensive training for those preparing or delivering the drug.
Application Area
Nothing illustrates 5-fluorouracil’s reach quite like its impact on global oncology. Standard of care for colorectal cancer? Check. Tool for basal cell carcinoma and actinic keratosis of the skin? Check again. Gynecological cancers, such as cervical and breast, count it as a trusty ally, especially before or after surgery. Used alone or in cocktail with other drugs — leucovorin, oxaliplatin, irinotecan — 5-FU forms the core of protocols like FOLFOX and FOLFIRI, still prescribed in leading cancer centers. Topically, dermatologists turn to 5-FU creams for stubborn skin lesions, putting mole-rat tenacity into treating precancerous and early cancers outside the operating room. Its versatility keeps it relevant even as new therapies surface.
Research & Development
The old dog keeps learning new tricks thanks to investment in R&D, where teams focus on two fronts: why some patients do better and how to make side effects less debilitating. Molecular biologists unravel the genetic codes that drive 5-FU metabolism; one key gene, DPD (dihydropyrimidine dehydrogenase), softens or intensifies the drug’s punch depending on a patient’s inherited makeup. Companies study new formulations — liposomal or nanoparticle variants — to direct 5-FU more precisely to tumor cells and keep damage away from healthy ones. Research teams also hunt for drug partners that boost 5-FU killing power or help cancer patients’ bodies recover faster. Continuous trials and pilot studies keep this workhorse relevant far beyond its mid-20th-century origins.
Toxicity Research
To anyone who’s sat through oncology training, the dark side of 5-FU looms large. Nausea, mouth sores, diarrhea, and dangerous suppression of white blood cells often come with therapy. At higher doses, confusion, seizures, and cardiac effects can appear. Much of this toxicity springs from both 5-FU and its byproducts affecting healthy cells that turn over quickly, such as those lining the gut or forming new blood. Research points to metabolic bottlenecks — especially DPD deficiency — that can make toxicity unpredictable or even lethal. Testing for metabolism rates, dose adjustments, and pre-treatment genetic screening gradually enter routine care. Supportive drugs, such as uridine triacetate, sometimes rescue patients from otherwise dire reactions, reflecting how hard clinicians work to balance cure and comfort.
Future Prospects
Despite the parade of new drugs, 5-fluorouracil stays relevant and shapes research into tomorrow’s cancer treatment. Teams look for gentler forms that can slip into nanoparticles, combining 5-FU with immune-stimulating molecules or local delivery patches that harness bioengineering. Artificial intelligence crunches patient genomics for clues about who will benefit most, or get hit hardest by side effects, so dosing gets smarter. Early signs suggest even long-standing drugs like 5-FU may regain lost ground against cancer’s ever-shifting genetics, especially if used together with checkpoint inhibitors or gene-editing therapies. Decades after its debut, 5-FU keeps raising new questions — a reminder that even the most familiar compounds can change lives in unexpected ways.
What is 5-Fluorouracil used for?
Cancer Treatment’s Familiar Face
Walk into an oncology ward and you will likely hear about 5-Fluorouracil, often called 5-FU. People battling cancer probably remember the name well after the infusions are over. Developed in the late 1950s, 5-FU remains a cornerstone for many types of cancers, especially those of the colon, rectum, breast, stomach, and pancreas. It is one of the most tried-and-tested drugs in chemotherapy, with decades of clinical experience backing its use. Ask any oncologist, and they usually have at least one patient currently on a 5-FU regimen.
My aunt fought colon cancer some years ago. Her journey through treatment involved regular 5-FU infusions, mixed with hope, dread, and conversations about what side effects might land hardest. Nurses explained that 5-FU attacks cells that grow fast—cancer cells grow out of control, so the drug stops them from copying their DNA and multiplying. That means the drug also affects other fast-growing cells in the body, like those in the lining of the mouth or the stomach, at the root of many side effects.
How 5-FU Works
5-FU acts as a sort of saboteur inside the body. It steps in for uracil, a building block that cancer cells need to create new copies of themselves. Once 5-FU sneaks in there, the cancer cell can’t make DNA properly, and the cell dies off. This isn’t gentle work—patients feel it. Mouth sores, lower resistance to infections, fatigue, and nausea are common. Many people also lose hair, deal with hand-and-foot syndrome, or notice a drop in appetite. Doctors always keep an eye on those side effects to balance the drug’s benefits with the toll it takes.
That tough balance matters. According to research published by the American Cancer Society, colon cancer survival rates improved significantly with chemotherapy, especially regimens including 5-FU. Before these treatments, the outlook for metastatic colon cancer was far bleaker. Now, five-year survival rates for early colon cancer have doubled in the last few decades, and 5-FU played no small part.
Outside of Cancer: Other Uses
Surprisingly, 5-FU reaches beyond treating cancer. Dermatologists use a cream form to handle actinic keratosis, those rough, scaly patches that sometimes show up after too much sun. Some precancerous skin conditions also respond well to a short course of 5-FU. The cream burns away abnormal skin cells and makes way for healthy cells. A few people find it tough to keep up the treatment because skin gets raw and flaky, but dermatologists often say better raw skin for a week than worries about skin cancer down the line.
Room for Progress and Solutions
For all the good it does, 5-FU still causes challenges. Some people break down 5-FU more slowly due to genetics, resulting in harsh side effects and, sometimes, hospitalization. Simple blood tests can spot these differences early. Insurance should support broad testing so folks know what they can safely tolerate. Drug companies work on safer, smarter forms of 5-FU or new combinations with supporting drugs that help shield normal cells or lessen side effects. My aunt’s doctor now offers options like cold caps for hair preservation and targeted drugs, but the old reliable 5-FU still plays a central role in many cancer cocktails.
At the heart of it, medicines like 5-FU shape stories—real lives, real heartbreak, and real hope. Improving how people handle these drugs means less suffering and a better path forward for patients and families caught in the cancer fight.
How is 5-Fluorouracil administered?
A Closer Look at the Journey
Many cancer patients hear the word “5-fluorouracil” from their oncologists and feel the usual swell of questions: How is this stuff delivered? What will my experience look like? Rather than crisp, official instructions from a pharmacy pamphlet, let’s reflect on how this drug becomes part of treatment—and how the way it’s given changes how people cope.
The Direct Route: Intravenous Delivery
Some intravenous drugs show up in an IV bag for a short burst, but 5-fluorouracil often takes a longer path. This chemo drug typically enters the system by a slow drip, threaded through a vein. That usually means a nurse connects an IV tube to a cannula set in the patient’s hand, arm, or sometimes through a more permanent line, such as a PICC (peripherally inserted central catheter) or a port.
I have watched friends undergo these infusions, and you notice quickly that it’s not just about the medicine but the time spent sitting, waiting, and chatting with others in the same boat. The slow infusion helps doctors control exposure and reduce severe reactions, which gives some peace of mind. For someone with a busy life, several hours at a clinic can be both a disruption and a forced moment to pause.
Pumps That Let You Go Home
Doctors sometimes offer portable infusion pumps, about the size of a small smartphone, so patients don’t have to stay hooked up to a machine in a hospital chair. The pump connects to the patient’s port or PICC, and he or she can go home with it, wearing it discreetly under clothing for a day or two.
This approach respects dignity and lets people cook, rest, or even walk the dog while chemo flows steadily into their veins. For many, this beats the alternative of repeated long sessions in a clinic. It still isn’t easy: changing dressings, checking for swelling, or spot signs of fever takes some effort. But that control means a lot.
Straight into the Belly: Special Circumstances
Surgeons sometimes deliver 5-fluorouracil right into the abdomen if cancer has spread around that area. This method, called intraperitoneal chemotherapy, usually blends surgery with treatment: doctors introduce the drug directly to where trouble lurks. This isn’t standard and comes with more discomfort, but in certain types of abdominal cancers, like those spreading from the colon or ovaries, local application improves the odds.
Swallowing a Pill—Rare, But Real
Swallowing chemo as a pill appeals, but 5-fluorouracil rarely works this way. The gut breaks down most of the drug before it can reach the bloodstream. Instead, doctors turn to oral alternatives, like capecitabine, which transforms into 5-fluorouracil inside the body. This option draws many preferences since it can be done at home, but it’s only suitable for specific cancers.
Making the Best Out of a Difficult Path
Many approaches exist because no two cancer cases match each other. Healthcare teams don’t simply choose based on science; they look at each person’s age, lifestyle, medical history, and even personal wishes. Frequent blood counts, as well as liver and kidney checks, help tailor the dose and schedule.
What’s clear from patient stories and oncology staff is that the “how” matters just as much as the “what.” Learning about these options gives people a sense of control and can ease some of the burden that comes with a cancer diagnosis. Progress in portable pumps and better oral medications holds hope for smoother days ahead.
What are the common side effects of 5-Fluorouracil?
5-Fluorouracil in Real-World Use
5-Fluorouracil, or 5-FU, gets prescribed often for certain cancers, such as those found in the colon, breast, and skin. Its reputation as a chemotherapy workhorse comes with reasons. It throws a wrench into the gears of cancer cell division, slowing or stopping their spread. Doctors and patients expect some turbulence during treatment, but it helps to know what real people actually face during a course of 5-FU.
Common Physical Setbacks
Many folks know about hair loss and nausea, but the experience feels different when it’s your own body. For a lot of people, mouth sores show up within a couple weeks of starting 5-FU. These aren’t just a passing irritation; eating and drinking anything acidic or spicy can turn into a major chore. Keeping ice chips handy sometimes helps, and doctors sometimes recommend rinsing with salt water.
Digestion tends to act up as well. Diarrhea often ranks among the most disruptive reactions. I’ve heard stories of patients suddenly needing to locate the nearest restroom even before finishing a meal. Severe bouts risk dehydration, so family and friends often keep electrolyte drinks stocked in the fridge. Constipation can show up as well but doesn’t carry the same reputation as diarrhea for this particular medication.
Nausea and vomiting sometimes hold center stage with any type of chemotherapy, and 5-FU is no exception. Recent data show modern anti-nausea medicines—ondansetron gets used a lot—help cut down on this misery, but they can’t always erase it. I’ve seen people pushed to try ginger candies, bland diets, and small frequent meals just to keep from losing too much weight or energy.
Changes in the Skin and Nails
5-FU can surprise people with odd effects on skin, fingers, and toes. Hand-foot syndrome shows up as redness, swelling, and even peeling. Some people find their fingertips grow numb or tingly, making buttoning a shirt tougher or turning pages a hassle. Bathing with cool water, avoiding harsh soaps, and comfortable shoes become small daily victories.
Rashes sometimes start with a mild itch but can progress to visible peeling or sores. Direct sunlight tends to make things worse, so doctors usually suggest covering up and generous use of sunscreen. Nails might darken or lift slightly from the nail bed—not exactly the most welcome sight.
How Blood Counts Drop
One thing people don’t always see coming: 5-FU can drop levels of white cells, red cells, or platelets. The body ends up with lower defenses against infections. I remember a neighbor postponing a family wedding visit because her neutrophil count looked shaky during her 5-FU cycles. Frequent lab checks and quick action at the first sign of fever can cut down on the risk.
Solutions and Looking Out for Each Other
Coping with these side effects means teamwork. Oncologists adjust doses or schedules depending on how the patient’s body copes. A nutritionist sometimes steps in, suggesting high-protein snacks or meal plans that soothe mouth sores. Nurses teach tricks for hand-foot syndrome—thick creams, soft socks, or rest during flare-ups. Friends and caregivers get trained to spot fevers, catch dehydration signs, and support someone through those rougher stretches.
Cancer treatment brings plenty of uncertainty, but good information and honest conversations help take the edge off. By sharing what 5-FU can throw at someone, people feel less alone and more prepared to handle both the expected and the surprises along the way.
Are there any precautions or contraindications with 5-Fluorouracil?
What 5-Fluorouracil Really Means for Patients
5-Fluorouracil gets prescribed for tough situations—mostly cancers like those of the colon, breast, and stomach. Skin creams with this drug tackle stubborn skin conditions, including certain pre-cancerous growths. Plenty of folks have family or friends bracing for these treatments. Medical teams rely on decades of research, but this drug demands close attention to patient safety from the start.
Risks Carry Weight for Certain Groups
Doctors always check for enzyme deficiencies—especially DPD (dihydropyrimidine dehydrogenase) deficiency—before the first dose. Without DPD, patients struggle to break down the drug, so toxic reactions can kick in. Severe mouth sores, diarrhea, and dangerous drops in white blood cells appear out of nowhere, leading to infections that spiral out of control. Blood tests help catch those at risk, but not every patient gets this screening. The hospital I once worked in saw a young man nearly lose his life to this hidden problem.
Pregnant women should avoid this medicine. Studies make it clear: the drug can harm unborn babies, especially during the earliest stages of pregnancy. It’s a tough call for families, but the evidence shows it’s not safe. Breastfeeding mothers also steer clear because the medicine can leak into breast milk.
People and Conditions Calling for Extra Caution
History of bone marrow suppression? This drug can push counts even lower. Infections can sneak up. Even people who get frequent sunburns or work outdoors see their risk of skin reactions climb. Anyone with liver or kidney disease runs the risk of slower drug clearance. Doctors adjust doses or sometimes choose different meds.
Sometimes, people take blood thinners like warfarin or certain seizure medications. Mixing these with 5-Fluorouracil multiplies the risks. You can’t just trust the pharmacy computer to catch every clash. In one case I saw, an older man landed in the ER with unstoppable bleeding, traced back to a drug interaction no one caught early on.
Monitoring Keeps People Safer
Close monitoring stands as the best protection. Frequent blood counts spot low platelets or infection early. Nausea, vomiting, and diarrhea definitely take their toll. Patients might believe side effects are something to push through. But telling the care team at every visit matters—a simple conversation about fatigue or new mouth sores sometimes prevents serious emergencies.
Labs aren’t the only tool. Family can notice confusion, fever, or trouble eating before it becomes a crisis. One patient told me their spouse caught a high fever fast—this quick reaction likely saved their life.
Improving Safety Together
Educating patients and families about early signs of trouble makes a huge difference. Hospitals with dedicated pharmacists checking drug interactions provide another safety net. Genetic testing isn’t universal yet, but the movement is growing. Every time a patient’s genetics get checked before treatment, one more life can stay on a safer path.
5-Fluorouracil isn’t for everyone. Every prescribing decision takes trust, up-to-date lab data, honest conversations, and teamwork from family, doctors, and pharmacists. That kind of vigilance gives patients the best shot at making it through difficult therapy on solid ground.
How should 5-Fluorouracil be stored?
Everyday Challenges in Handling Chemotherapy Drugs
Dealing with cancer forces a person to trust a whole chain of hands, from the pharmacist behind the counter to the oncology nurse prepping an IV. There’s no room for careless mistakes. 5-Fluorouracil (also called 5-FU) has been part of chemotherapy treatments for decades. Its power and danger run side by side. That’s why safe storage can’t be an afterthought. Watching my great-uncle go through rounds of cancer care, it became clear that any slip-up—whether in mixing or storage—could mean the difference between relief and catastrophe.
Keeping It Cold and Out of Sight
Doctors and nurses don’t lock up 5-FU in a cold spot just because they feel like it. This drug breaks down if left sitting in the warmth or sunlight. Pharmacies store it at temperatures between 2°C to 8°C, the sweet spot for refrigerators. Once outside these conditions, 5-FU starts losing its punch, which puts patients at risk. I learned during pharmacy school that keeping medications like this in a regular kitchen fridge at home just doesn’t cut it. Home storage brings risk from temperature swings every time someone grabs the milk, and that can be enough for a sensitive compound like 5-FU to lose stability.
Practical Risks of Poor Storage
Consider the statistics. Studies warned that cytotoxic drugs like 5-FU degrade fast if exposed to light or heat. Storage outside its safe range lets breakdown products form, which either weaken the dose or, worse, cause unexpected side effects. In most cancer centers, the chemo drugs get a special section in coolers or pharmacy fridges, protected from both heat and prying eyes. No one wants a child or an untrained staff member stumbling across this vial by accident.
Handling Safety for Staff and Patients
Those who handle 5-FU every day—like nurses mixing solutions or pharmacists counting vials—stand in the crosshairs of workplace safety. The drug is toxic to more than cancer cells, and direct contact can harm skin or eyes. I remember a nurse sharing stories of accidents, some avoidable, some freakish. They always came back to this: Safe storage means less chaos, fewer burns and fewer rushed trips to the emergency room.
Maintaining Accountability with Clear Procedures
Hospitals and clinics use tight controls for good reasons. Pharmacies keep logs of every vial stored and every dose dispensed. Smart inventory systems alert staff when temperatures go outside the safe range. There’s a lesson for smaller offices and home care too—if you can’t guarantee a safe, monitored fridge, don’t keep the vials at home. In my own small-town pharmacy, we’ve invested in backup power for our medical fridge. Power outages happen, and nothing feels worse than losing expensive chemo drugs—and risking lives—over something avoidable.
Ideas for a Safer Future
Some newer formulations of 5-FU extend shelf life without refrigeration, but those products stay rare and expensive. Until better solutions reach every clinic, the old rules matter. Keep 5-FU refrigerated. Protect it from light. Lock it away from the wrong hands. Sometimes simple vigilance saves lives and spares families the terrible consequences of careless mistakes. For anyone involved with this drug, from pharmacists to caregivers at home, nothing replaces a clear-eyed focus on safety and proper storage.
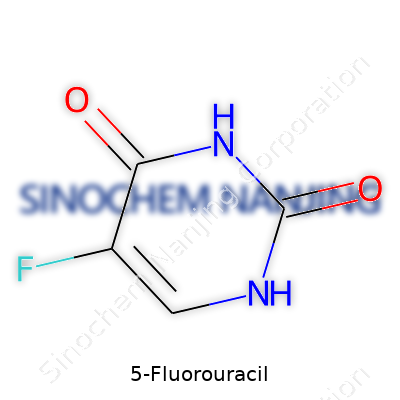
| Names | |
| Preferred IUPAC name | 5-fluoro-1H-pyrimidine-2,4-dione |
| Other names |
Adrucil Efudex Fluoroplex Carac 5-FU |
| Pronunciation | /faɪˌfluː.roʊˈjʊə.rə.sɪl/ |
| Identifiers | |
| CAS Number | 51-21-8 |
| Beilstein Reference | 172059 |
| ChEBI | CHEBI:9517 |
| ChEMBL | CHEMBL1431 |
| ChemSpider | 38853 |
| DrugBank | DB00544 |
| ECHA InfoCard | 03d076ad-9af6-47e4-b271-001cfc0eecab |
| EC Number | EC 206-398-3 |
| Gmelin Reference | **83254** |
| KEGG | C00485 |
| MeSH | D005473 |
| PubChem CID | 3385 |
| RTECS number | YO6300000 |
| UNII | O66KB9A8DV |
| UN number | 2811 |
| Properties | |
| Chemical formula | C4H3FN2O2 |
| Molar mass | 130.08 g/mol |
| Appearance | White to practically white, crystalline powder |
| Odor | Odorless |
| Density | 1.325 g/cm³ |
| Solubility in water | 8.2 g/L (at 25 °C) |
| log P | -0.89 |
| Vapor pressure | 4.01E-8 mmHg at 25°C |
| Acidity (pKa) | 8.0 |
| Basicity (pKb) | 11.15 |
| Magnetic susceptibility (χ) | Diamagnetic |
| Refractive index (nD) | 1.469 |
| Viscosity | Viscous liquid |
| Dipole moment | 4.20 D |
| Thermochemistry | |
| Std molar entropy (S⦵298) | 166.5 J·mol⁻¹·K⁻¹ |
| Std enthalpy of formation (ΔfH⦵298) | -531.7 kJ/mol |
| Std enthalpy of combustion (ΔcH⦵298) | -2929 kJ/mol |
| Pharmacology | |
| ATC code | L01BC02 |
| Hazards | |
| Main hazards | May cause cancer; Causes serious eye irritation; May cause an allergic skin reaction; Toxic if swallowed, in contact with skin or if inhaled |
| GHS labelling | GHS07, GHS08 |
| Pictograms | GHS06,GHS08 |
| Signal word | Danger |
| Hazard statements | H301, H315, H319, H351, H360, H373 |
| Precautionary statements | P201, P202, P261, P272, P280, P308+P313, P405, P501 |
| NFPA 704 (fire diamond) | 1-2-0 |
| Lethal dose or concentration | LD50 oral rat 230 mg/kg |
| LD50 (median dose) | LD50 (median dose): Mouse (oral) 245 mg/kg |
| NIOSH | NIOSH: Y0000657 |
| PEL (Permissible) | Not established |
| REL (Recommended) | REL (Recommended): 2 mg/m³ |
| IDLH (Immediate danger) | Unknown |
| Related compounds | |
| Related compounds |
Uracil Flucytosine Capecitabine Tegafur Carmofur Eniluracil |